Scientists have shown in mice that skin cells re-programmed into brain stem cells, transplanted into the central nervous system, help reduce inflammation and may be able to help repair damage caused by multiple sclerosis (MS).
Our mouse study suggests that using a patient’s reprogrammed cells could provide a route to personalised treatment of chronic inflammatory diseases, including progressive forms of MS
Luca Peruzzotti-Jametti
The study, led by researchers at the University of Cambridge, is a step towards developing personalised treatments based on a patient’s own skin cells for diseases of the central nervous system (CNS).
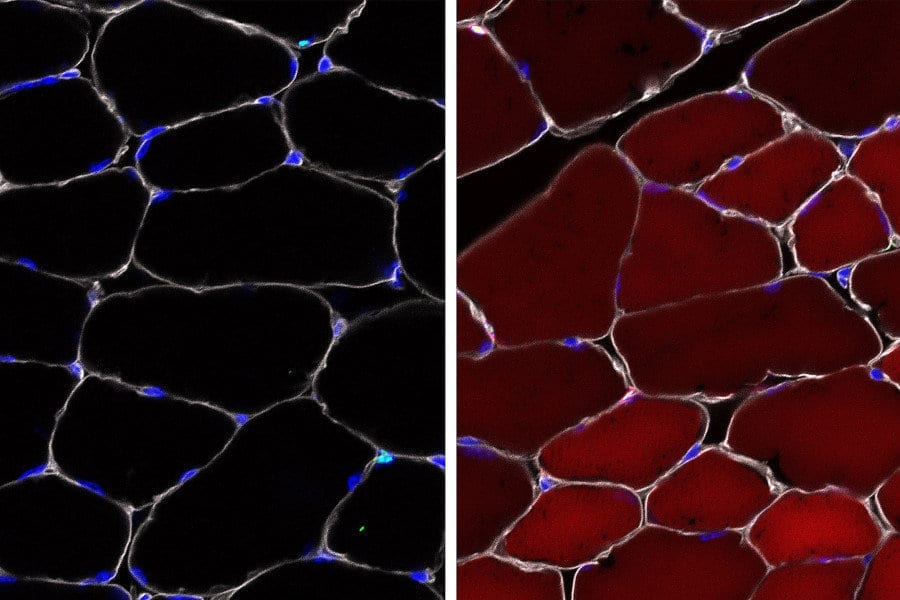
In MS, the body’s own immune system attacks and damages myelin, the protective sheath around nerve fibres, causing disruption to messages sent around the brain and spinal cord. Symptoms are unpredictable and include problems with mobility and balance, pain, and severe fatigue.
Key immune cells involved in causing this damage are macrophages (literally ‘big eaters’), which ordinarily serve to attack and rid the body of unwanted intruders. A particular type of macrophage known as microglia are found throughout the brain and spinal cord – in progressive forms of MS, they attack the CNS, causing chronic inflammation and damage to nerve cells.
Recent advances have raised expectations that diseases of the CNS may be improved by the use of stem cell therapies. Stem cells are the body’s ‘master cells’, which can develop into almost any type of cell within the body. Previous work from the Cambridge team has shown that transplanting neural stem cells (NSCs) – stem cells that are part-way to developing into nerve cells – reduces inflammation and can help the injured CNS heal.
However, even if such a therapy could be developed, it would be hindered by the fact that such NSCs are sourced from embryos and therefore cannot be obtained in large enough quantities. Also, there is a risk that the body will see them as an alien invader, triggering an immune response to destroy them.
A possible solution to this problem would be the use of so-called ‘induced neural stem cells (iNSCs)’ – these cells can be generated by taking an adult’s skin cells and ‘re-programming’ them back to become neural stem cells. As these iNSCs would be the patient’s own, they are less likely to trigger an immune response.
Now, in research published in the journal Cell Stem Cell, researchers at the University of Cambridge have shown that iNSCs may be a viable option to repairing some of the damage caused by MS.
Using mice that had been manipulated to develop MS, the researchers discovered that chronic MS leads to significantly increased levels of succinate, a small metabolite that sends signals to macrophages and microglia, tricking them into causing inflammation, but only in cerebrospinal fluid, not in the peripheral blood.
Transplanting NSCs and iNSCs directly into the cerebrospinal fluid reduces the amount of succinate, reprogramming the macrophages and microglia – in essence, turning ‘bad’ immune cells ‘good’. This leads to a decrease in inflammation and subsequent secondary damage to the brain and spinal cord.
“Our mouse study suggests that using a patient’s reprogrammed cells could provide a route to personalised treatment of chronic inflammatory diseases, including progressive forms of MS,” says Dr Stefano Pluchino, lead author of the study from the Department of Clinical Neurosciences at the University of Cambridge.
“This is particularly promising as these cells should be more readily obtainable than conventional neural stem cells and would not carry the risk of an adverse immune response.”
The research team was led by Dr Pluchino, together with Dr Christian Frezza from the MRC Cancer Unit at the University of Cambridge, and brought together researchers from several university departments.
Dr Luca Peruzzotti-Jametti, the first author of the study and a Wellcome Trust Research Training Fellow, says: “We made this discovery by bringing together researchers from diverse fields including regenerative medicine, cancer, mitochondrial biology, inflammation and stroke and cellular reprogramming. Without this multidisciplinary collaboration, many of these insights would not have been possible.”
Learn more: Study in mice suggests personalised stem cell treatment may offer relief for progressive MS
The Latest on: Personalised stem cell treatment
[google_news title=”” keyword=”Personalised stem cell treatment” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]
via Google News
The Latest on: Personalised stem cell treatment
- How AI is boosting cancer treatmenton May 18, 2024 at 1:29 am
Treatment of cancers is no longer just limited to traditional approaches like chemotherapy, radiation, and surgery. Artificial intelligence (AI) is making significant strides in cancer treatment ...
- New cancer research enables better immunotherapy treatmenton May 15, 2024 at 5:00 pm
they can gain additional insights that will help tailor personalized treatment plans. The breakthrough, made by a team at Bar-Ilan University (BIU), allows clinicians to better understand the complex ...
- Stem Cell Therapy Accelerates Recovery for Ferrari Challenge Driver Marco Pulcinion May 14, 2024 at 9:37 pm
The advanced technology means Pulcini can return to his regular racing itinerary stronger and fitter than ever.Bogota, Colombia - May 15, 2024 ...
- Brain Cancer Awareness Month: Challenges and Innovations in Treatmenton May 14, 2024 at 10:31 am
In an interview with Targeted Oncology for Brain Cancer Awareness Month, Theodore Schwartz, MD, discussed the challenges of targeting brain tumors, emerging therapies, and strategies to overcome the ...
- Peak Health Group Champions Holistic Patient Care through Advanced IV Therapy Serviceson May 13, 2024 at 9:15 am
Peak Health Group revolutionizes healthcare with its cutting-edge IV therapy offerings, providing personalized solutions for optimizing health ...
- Study Finds Opportunities for Personalized Glioblastoma Treatmenton May 13, 2024 at 2:41 am
Proteogenomic analysis of glioblastoma recurrence has offered potential new therapeutic avenues and opportunities for personalized treatment.
- Korea University College of Medicine’s team facilitates personalized treatment opportunities for malignant brain tumor, glioblastomaon May 9, 2024 at 4:59 pm
Longitudinal proteogenomic analysis reveals increased neuronal state at recurrence • Neuronal transition associates with activation of WNT/PCP pathway and BRAF kinase • Resistance to therapy via neuro ...
- Adding immune-boosting agent to personalized cancer vaccine supercharges the body's immune defense against malignant brain tumorson May 9, 2024 at 9:18 am
Investigators at the UCLA Health Jonsson Comprehensive Cancer Center have pinpointed a combination immunotherapy treatment that enhances the immune response for people with malignant gliomas, an ...
- Immune cell discovery ‘could lead to personalised treatment for breast cancer’on May 7, 2024 at 10:32 pm
Scientists have found that some immune cells hunt down cancer in the body, a discovery that could lead to personalised treatments for advanced breast cancer. The study identified features of cells ...
- AI-driven model identifies potent cancer-killing immune cells for personalized immunotherapyon May 7, 2024 at 9:46 pm
Using artificial intelligence, Ludwig Cancer Research scientists have developed a powerful predictive model for identifying the most potent cancer killing immune cells for use in cancer ...
via Bing News