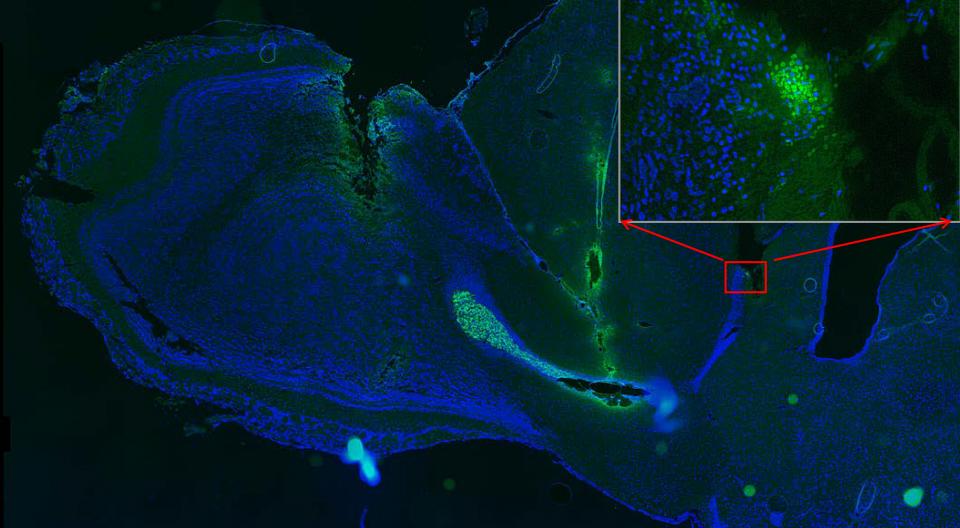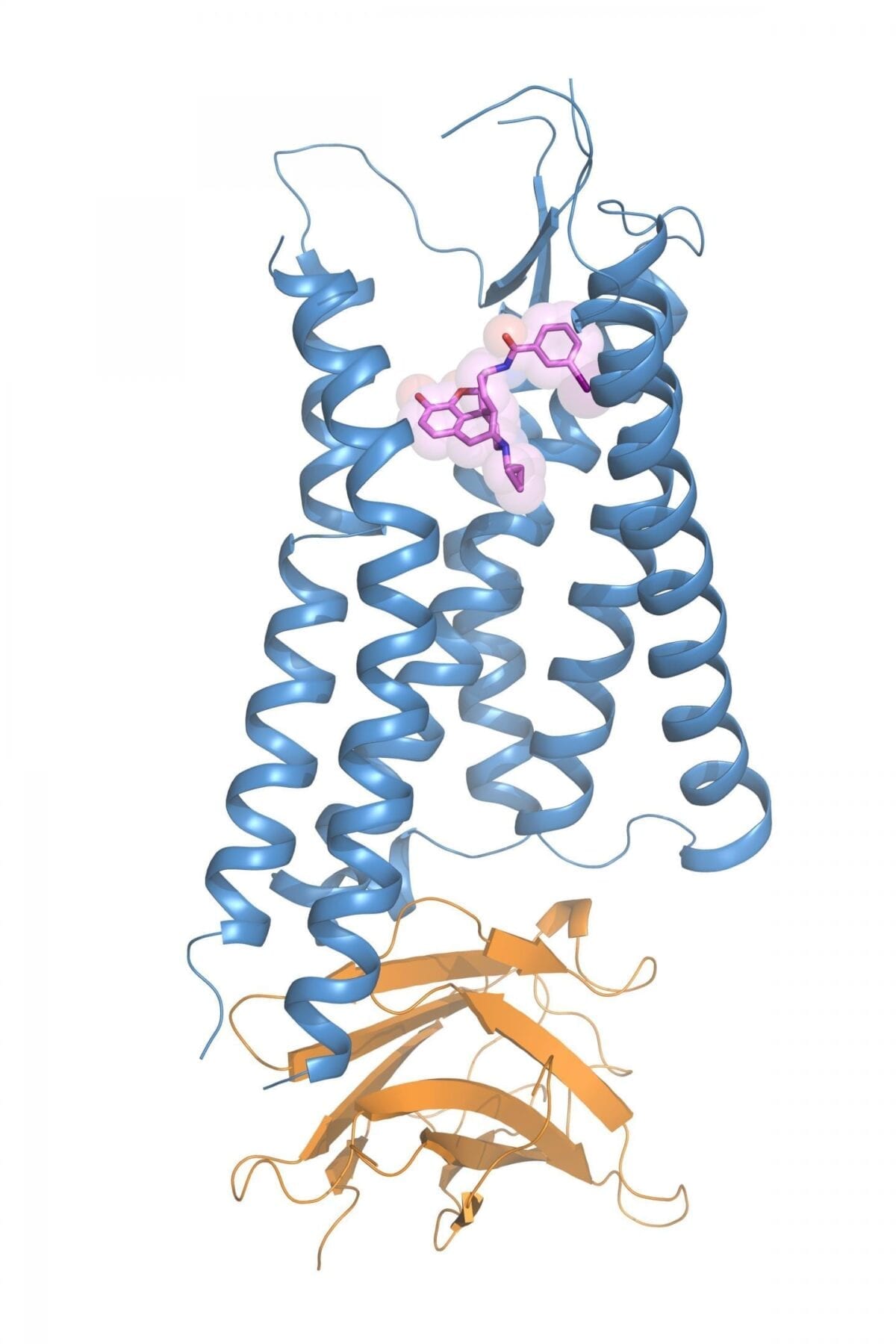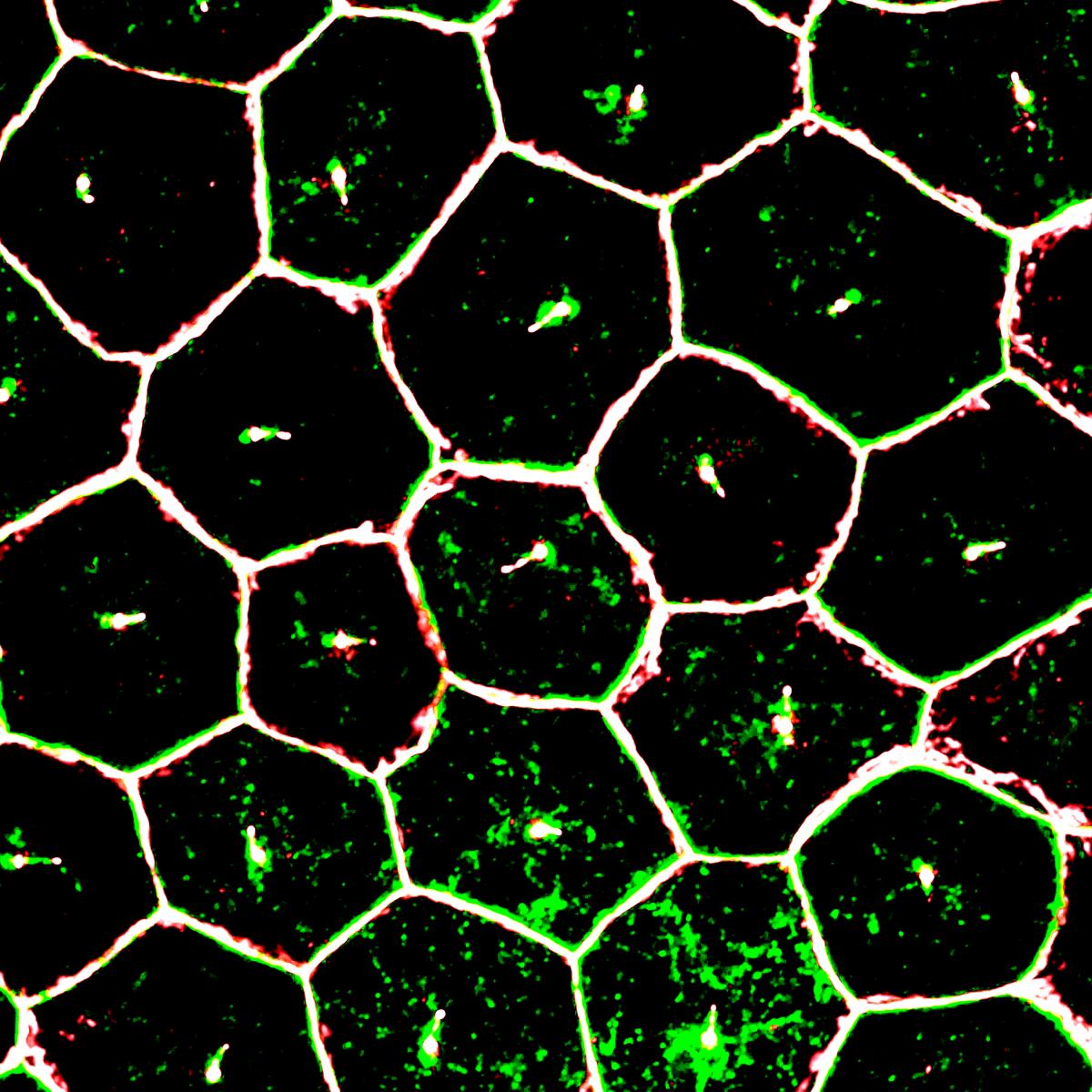
tight junction markers. Credit: Ruchi Sharma, Ph.D., NEI.
Stem cell-derived retinal cells need primary cilia to support survival of light-sensing photoreceptors
Scientists at the National Eye Institute (NEI), part of the National Institutes of Health, report that tiny tube-like protrusions called primary cilia on cells of the retinal pigment epithelium (RPE)—a layer of cells in the back of the eye—are essential for the survival of the retina’s light-sensing photoreceptors. The discovery has advanced efforts to make stem cell-derived RPE for transplantation into patients with geographic atrophy, otherwise known as dry age-related macular degeneration (AMD), a leading cause of blindness in the U.S. The study appears in the January 2 Cell Reports.
“We now have a better idea about how to generate and replace RPE cells, which appear to be among the first type of cells to stop working properly in AMD,” said the study’s lead investigator, Kapil Bharti, Ph.D., Stadtman investigator at the NEI. Bharti is leading the development of patient stem cell-derived RPE for an AMD clinical trial set to launch in 2018.
In a healthy eye, RPE cells nourish and support photoreceptors, the cells that convert light into electrical signals that travel to the brain via the optic nerve. RPE cells form a layer just behind the photoreceptors. In geographic atrophy, RPE cells die, which causes photoreceptors to degenerate, leading to vision loss.
Bharti and his colleagues are hoping to halt and reverse the progression of geographic atrophy by replacing diseased RPE with lab-made RPE. The approach involves using a patient’s blood cells to generate induced-pluripotent stem cells (iPSCs), cells capable of becoming any type of cell in the body. iPSCs are grown in the laboratory and then coaxed into becoming RPE for surgical implantation.
Attempts to create functional RPE implants, however, have hit a recurring obstacle: iPSCs programmed to become RPE cells have a tendency to get developmentally stuck, said Bharti. “The cells frequently fail to mature into functional RPE capable of supporting photoreceptors. In cases where they do mature, however, RPE maturation coincides with the emergence of primary cilia on the iPSC-RPE cells.”
The researchers tested three drugs known to modulate the growth of primary cilia on iPSC-derived RPE. As predicted, the two drugs known to enhance cilia growth significantly improved the structural and functional maturation of the iPSC-derived RPE. One important characteristic of maturity observed was that the RPE cells all oriented properly, correctly forming a single, functional monolayer. The iPSC-derived RPE cell gene expression profile also resembled that of adult RPE cells. And importantly, the cells performed a crucial function of mature RPE cells: they engulfed the tips of photoreceptor outer segments, a pruning process that keeps photoreceptors working properly.
By contrast, iPSC-derived RPE cells exposed to the third drug, an inhibitor of cilia growth, demonstrated severely disrupted structure and functionality.
As further confirmation of their observations, when the researchers genetically knocked down expression of cilia protein IFT88, the iPSC-derived RPE showed severe maturation and functional defects, as confirmed by gene expression analysis. Tissue staining showed that knocking down IFT88 led to reduced iPSC-derived RPE cell density and functional polarity, i.e., cells within the RPE tissue pointed in the wrong direction.
Bharti and his group found similar results in iPSC-derived lung cells, another type of epithelial cell with primary cilia. When iPSC-derived lung cells were exposed to drugs that enhance cilia growth, immunostaining confirmed that the cells looked structurally mature.
The report suggests that primary cilia regulate the suppression of the canonical WNT pathway, a cell signaling pathway involved in embryonic development. Suppression of the WNT pathway during RPE development instructs the cells to stop dividing and to begin differentiating into adult RPE, according to the researchers.
The researchers also generated iPSC-derived RPE from a patient with ciliopathy, a disorder that causes severe vision loss due to photoreceptor degeneration. The patient’s ciliopathy was associated with mutations of cilia gene CEP290. Compared to a healthy donor, iPSC-derived RPE from the ciliopathy patient had cilia that were smaller. The patient’s iPSC-derived RPE also had maturation and functional defects similar to those with IFT88 knockdown.
Further studies in a mouse model of ciliopathy confirmed an important temporal relationship: Looking across several early development stages, the RPE defects preceded the photoreceptor degeneration, which provides additional insights into ciliopathy-induced retinal degeneration.
Learn more: NIH discovery brings stem cell therapy for eye disease closer to the clinic
The Latest on: Dry age-related macular degeneration
[google_news title=”” keyword=”dry age-related macular degeneration” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]- Tips to Make Working Easier With Wet Age-Related Macular Degenerationon May 2, 2024 at 5:00 pm
If dry AMD develops into the wet form ... can be very helpful for patients suffering from vision loss from macular degeneration,” he says. “They allow you to maximize the vision you have ...
- Macular Degeneration: 11 Ways to Protect Your Eyeson May 2, 2024 at 9:17 am
It is crucial to be aware of the risk factors and symptoms associated with AMD to detect and manage the condition early.
- What Is Wet Age-Related Macular Degeneration?on May 1, 2024 at 5:00 pm
To help detect or confirm a diagnosis of wet AMD, your doctor may perform other tests and procedures, including the following: Both dry and wet age-related macular degeneration (AMD) involve ...
- Dry Age-related Macular Degeneration Seven Major Market to Exhibit Growth at a CAGR of 19.8% by 2034 | DelveInsighton April 22, 2024 at 2:31 pm
Dry Age-related Macular Degeneration Pipeline Insight – 2024 report provides comprehensive insights about the pipeline landscape, pipeline drug profiles, including clinical and non-clinical ...
- Dry Age-related Macular Degeneration Seven Major Market to Exhibit Growth at a CAGR of 19.8% by 2034 | DelveInsighton April 22, 2024 at 2:31 pm
DelveInsight's Dry Age-related Macular Degeneration Market Insights report includes a comprehensive understanding of current treatment practices, dry age-related macular degeneration marketed drug, ...
- Neovascular Age-Related Macular Degenerationon April 17, 2024 at 5:00 pm
Choroidal neovascularization is the primary cause of visual loss in patients with age-related macular degeneration. Current treatments, proven to offer a benefit for these patients through ...
- Atrophic macular degeneration: What to knowon April 15, 2024 at 5:00 pm
Atrophic macular degeneration, or geographic atrophy, is an advanced stage of dry age-related macular degeneration. Destruction of the cells — known as atrophy — in the retina can eventually ...
- Wet vs. Dry Macular Degeneration: What Is the Difference?on April 14, 2024 at 5:00 pm
Both types of age-related macular degeneration (AMD) can cause blurriness and visual changes. Dry AMD progresses slowly and causes permanent damage, while wet AMD is more severe but more treatable.
via Google News and Bing News