Credit: James Gathany/CDC
When it comes to early diagnosis of Lyme disease, the insidious tick-borne illness that afflicts about 300,000 Americans annually, finding the proverbial needle in the haystack might be a far easier challenge—until now, perhaps. An experimental method developed by federal and university researchers appears capable of detecting the stealthy culprit Lyme bacteria at the earliest time of infection, when currently available tests are often still negative.
The team suggests the approach might also be useful for early detection of other elusive bacterial infections. The collaborators—from the National Institute of Standards and Technology (NIST), Institute for Bioscience and Biotechnology Research, and Johns Hopkins School of Medicine—recently reported the successful first trial of their new method.
“Our hypothesis was that Lyme bacteria shed vesicle-like particles—or fragments—derived from the cell wall of the bacteria circulating in the serum of individuals. These particles would contain membrane proteins that can be detected to provide a unique indicator of infection,” explains NIST research chemist Larik Turko.
The challenge was to detect these bacterial membrane proteins among the far, far more plentiful proteins normally present in serum, the watery, cell-free component of blood. The researchers speculated that running serum samples through a high-speed centrifuge—a standard step in chemistry labs—might selectively concentrate the larger, heavier fragments containing the bacterial membrane proteins into pellets. In effect, they predicted, this step would separate the wheat—the sparse target proteins—from the chaff—the much more abundant human serum proteins.
The new method’s promise was demonstrated in tests on serum samples drawn from three patients with undetected Lyme disease at the time of their initial doctor visit. By customizing standard analytical techniques for determining the types and amounts of chemicals in a sample, the team detected extremely small amounts of the target protein in all three samples.
For chemistry buffs, the protein in enriched samples was present at a level of about four billionths of a millionth of a mole, the standard unit for amount of substance.
In one patient, the experimental method detected the bacteria three weeks before infection was confirmed with the standard blood tests now used. For the other two, infection was detected simultaneously by the two methods.
“The complexity of Lyme disease, combined with lack of biomarkers to measure infection, has slowed progress,” study collaborator John Aucott, head of the Johns Hopkins Lyme Disease Clinical Research Center, said in advance of a session on precision and personalized medicine this weekend at the AAAS 2016 Annual Meeting in Washington, D.C. “Now, thanks to recent advances in technology, the tiniest concentration of blood molecules can now be detected, molecules that were previously ‘invisible’ to scientists.”
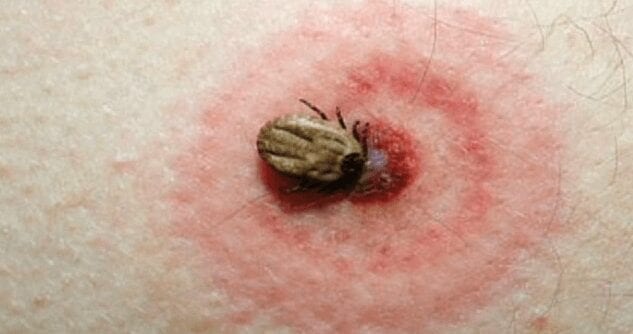
The current standard blood test for Lyme disease exposes the infection only after antibodies have accumulated to detectable levels, which can take up to 4 to 6 weeks. If patients exhibit a telltale bull’s-eye rash, diagnosis and treatment can begin earlier. But the rash does not occur in 20 to 30 percent of Lyme disease patients, according to the Centers for Disease Control and Prevention.
Rather than waiting for an infected person’s immune system to produce noticeable amounts of antibodies, the team chose to home in on the bacteria itself—specifically, proteins the bug sheds when attacked by the body’s defenses.
“From many candidates, we chose one that is both easily distinguished from human serum proteins and an unambiguous indicator of the bacteria,” Turko says. “This protein, which resides on the outer surface of membranes, became the target of our search in serum samples.”
But finding that target required an important preliminary step to ensure the accuracy of their measurements: making a reference sample that contained ample amounts of the target protein. With the reference sample, the team established the unmistakable signature the bug’s outer-surface membrane protein would yield when they examined samples drawn from patients. As a result of these steps, the team could detect the copies of the target protein, even though human proteins were 10 million times more plentiful.
“We believe that this approach may be universally applicable to detection of other bacterial infections in humans,” the researchers write.
Learn more: New Experimental Test Detects Signs of Lyme Disease Near Time of Infection
The Latest on: Lyme disease
[google_news title=”” keyword=”Lyme disease” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]
via Google News
The Latest on: Lyme disease
- Dog owners issued Lyme Disease and tick warning by veton May 3, 2024 at 2:17 pm
But spending more time among nature means a heightened risk of tick bites, which can, in some cases, result in Lyme disease. Dr Hannah Godfrey, vet at Petsure, warned: “You can recognise a tick by ...
- Lyme disease: It only takes one biteon May 3, 2024 at 10:30 am
I'm a strong, well-trained former pro athlete. How could an opponent as tiny as a tick defeat me? Because Lyme disease is real. I've battled it for decades. The pernicious, insidious disease — hard to ...
- Spring is time to combat Lyme disease and other tick-borne diseaseson May 3, 2024 at 9:59 am
While ticks are most active in spring and summer, they can be found during any time of the year when the temperature is above freezing ...
- Expert warns of Lyme disease risk in South Georgiaon May 3, 2024 at 7:48 am
May 1—TIFTON — As the weather warms and more people venture outside, Abraham Baldwin Agricultural College professor Tony Matthews cautions that Lyme disease remains a concern for those exploring ...
- Mom’s memory loss and tingling were dismissed by 14 doctors. It was neurologic Lyme diseaseon May 3, 2024 at 6:54 am
Kirsten Stein panicked when she couldn't find her son. She forgot she had just dropped him off at school. Her new symptoms were a sign of Lyme disease.
- Researchers launching tick study after record year for Lyme diseaseon May 2, 2024 at 5:00 pm
The state already has recorded 261 Lyme disease cases this year. The University of Maine will launch a pilot program this month to better understand tick populations on the heels of a record-setting ...
- What It’s Like to Live With Neurologic Lyme Disease: A Patient Perspectiveon April 30, 2024 at 5:00 pm
Credit: Getty Images Diagnosing patients with neurologic Lyme disease can take upwards of 2 years, which Maria Arini Lopez discovered first-hand in the spring of 2021. Lyme Disease Awareness Month ...
- Is Lyme disease curable? Here's what you should know about tick bites and symptoms.on April 30, 2024 at 4:37 am
For most people, Lyme disease is cured with 2-4 weeks worth of antibiotics. However, some people may have lingering damage and symptoms.
- As ticks spread, the US is getting smart about reporting infections and seeing the true extent of Lyme diseaseon April 28, 2024 at 3:43 pm
The Centers for Disease Control and Prevention — the federal agency that monitors diseases and establishes guidelines to protect human health — published a paper in February that shows cases of Lyme ...
- How Is Lyme Disease Treated?on April 27, 2024 at 10:00 am
Lyme disease is a bacterial illness spread by deer ticks. Antibiotics are the primary Lyme disease treatment, but home remedies can help.
via Bing News