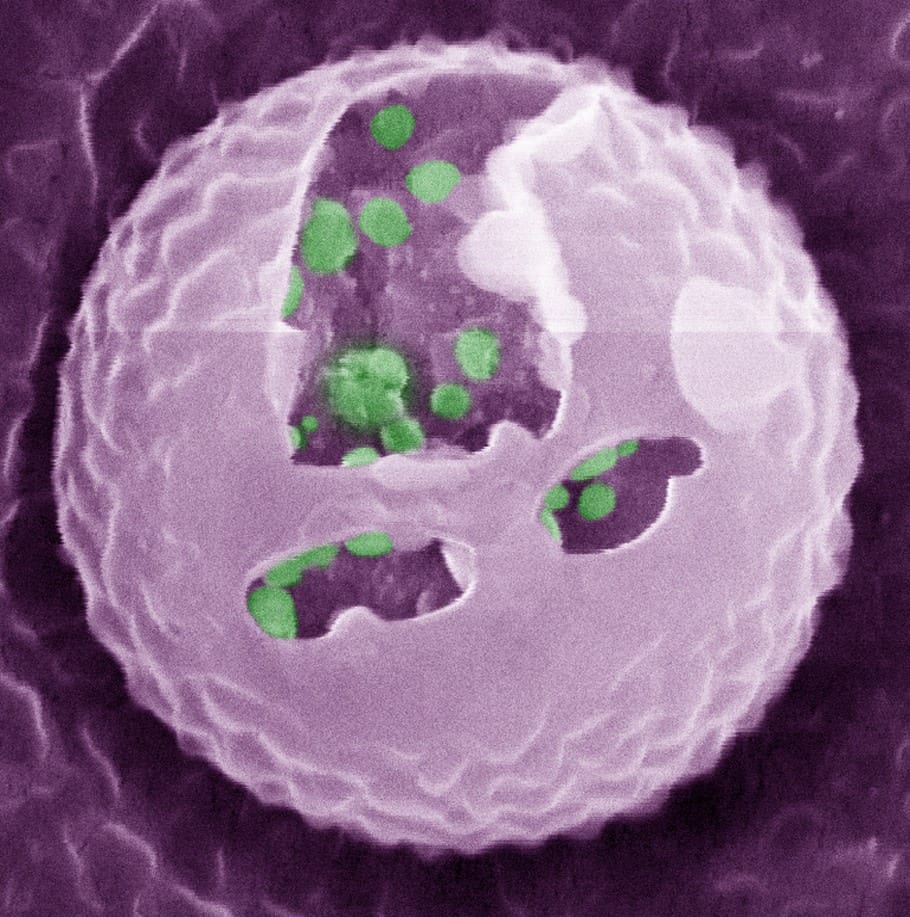
In lab experiments and animal models, UNC and NC State researchers led by Zhen Gu, PhD, designed synthetic beta cells to secrete insulin in response to high blood sugar.
Treating type 1 diabetes and some cases of type 2 diabetes has long required painful and frequent insulin injections or a mechanical insulin pump for insulin infusion. But researchers from the University of North Carolina and NC State have now developed what could be a much more patient-friendly option: artificial cells that automatically release insulin into the bloodstream when glucose levels rise.
These “artificial beta cells” (A?Cs) mimic the functions of the body’s natural glucose-controllers, the insulin-secreting beta cells of the pancreas. The loss or dysfunction of these cells causes type 1 diabetes and many cases of type 2 diabetes. The idea is that the A?Cs could be subcutaneously inserted into patients, which would be replaced every few days, or by a painless and disposable skin patch.
As the researchers report in Nature Chemical Biology, a single injection of the A?Cs into diabetic mice lacking beta cells quickly normalized the animals’ blood glucose levels and kept those levels normal for up to five days.
“Our plan now is to further optimize and test these synthetic cells in larger animals, develop a skin patch delivery system for them, and ultimately test them in people with diabetes,” said principal investigator Zhen Gu, PhD, a professor in the Joint UNC/NC State Department of Biomedical Engineering. Gu also holds appointments in the UNC School of Medicine, the UNC Eshelman School of Pharmacy, and the UNC Diabetes Care Center.
At least six million people in the United States use insulin as a diabetes treatment, either by injection or a mechanical pump. So far, delivered insulin in pill form has been challenging because it’s a large molecule that would be destroyed by digestive enzymes and acids before it could reach the bloodstream.
The major problem with current insulin treatments, however, is not that they can’t be delivered in a pill, but that they can’t control blood glucose levels automatically and efficiently, as normal insulin-secreting pancreatic cells do. Transplants of pancreatic cells can solve that problem in some cases. However, such cell transplants are expensive, require donor cells that are often in short supply, require immune-suppressing drugs, and often fail due to the destruction of the transplanted cells.

- False color Cryo-Scanning Electron Microscope image of the artificial beta cells. (Gu Lab, UNC-NC State)
Gu and colleagues have been researching solutions to the insulin-delivery problem for much of the past decade. For this project, they adopted a particularly ambitious approach: making artificial cells that, to a great extent, do what natural pancreatic beta cells do.
Gu’s A?Cs are constructed with a simplified version of a normal cell’s two-layered lipid membrane. The key innovation is what these cells contain: specially designed, insulin-stuffed vesicles. A rise in blood glucose levels leads to chemical changes in the vesicle coating, causing the vesicles to start fusing with the A?C’s outer membrane – thus releasing the insulin payloads.
“This is the first demonstration using such a vesicle fusion process for delivering insulin that employs insulin-containing vesicles like those found in a beta cell and can reproduce the beta cell’s functions in sensing glucose and responding with insulin ’secretion’,” said Zhaowei Chen, PhD, a lead author and postdoctoral researcher in Gu’s lab.
The A?Cs showed a rapid responsiveness to excess glucose levels in lab-dish tests and in diabetic mice without beta cells. “The mice went from hyperglycemic to normoglycemic within an hour, and they remained normoglycemic for up to five days after that,” Gu said. Control mice injected with no-insulin A?Cs remained hyperglycemic.
Gu and colleagues plan further preclinical tests and expect to develop a method for delivering the cells painlessly via a skin patch that could be simply replaced.
Co-author John Buse, MD, PhD, the Verne S. Caviness Distinguished Professor at UNC, chief of the division of endocrinology, and director of the UNC Diabetes Care Center, said, “There is still much work needed to optimize this artificial-cell approach before human studies are attempted, but these results so far are a remarkable, creative first step to a new way to solve the diabetes problem using chemical engineering as opposed to mechanical pumps or living transplants.”
Gu and his team are also working separately on a cell-free skin patch, a “smart insulin patch” that senses blood glucose levels and secretes insulin into the bloodstream as needed.
Learn more: Smart Artificial Beta Cells Could Lead to New Diabetes Treatment
The Latest on: Synthetic beta cells
[google_news title=”” keyword=”Synthetic beta cells” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]- Century Therapeutics Presents Preclinical Data Highlighting Advances in iPSC Platform Technology and Programs at 2024 ASGCT Annual Meetingon May 10, 2024 at 5:59 am
In vitro data showcases CNTY-101’s ability to induce CD19-specific cytolysis of B-cells and potential to treat B-cell driven autoimmune diseases ...
- CorePeptides Unveils Breakthrough Palmitoyl Tripeptide Researchon May 9, 2024 at 12:06 am
CorePeptides Unveils Breakthrough Palmitoyl Tripeptide Research. New York, USA - May 9, 2024 — Synthetic peptides with anti-aging action on the cell cycles are abundant in research studies; one such ...
- Cell therapy fails to slow early type 1 diabetes, but safety is establishedon May 8, 2024 at 11:00 am
Despite the negative finding, researchers said there is still promise in the strategy of amplifying and infusing the immune cells of newly diagnosed type 1 diabetes patients.
- MIT Technology Reviewon May 5, 2024 at 5:00 pm
The experiment, at the University of Florida, is an attempt to create a large animal starting only from stem cells—no egg, no sperm, and no conception. A week earlier, “synthetic embryos ...
- Engineering Life: Chemists Have Created the Functional Synthetic Cells That Act Like Real Oneson May 3, 2024 at 6:10 pm
Researchers employ cutting-edge methods to create functional cells, closing the divide between synthetic and biological materials. In a new study published in Nature Chemistry, UNC-Chapel Hill researc ...
- Synthetic Cells That Mimic Biology Could Offer Clues on Mysteries of Life, its Origins, and Extraterrestrialson May 3, 2024 at 10:31 am
Scientists say they are making progress in the development of synthetic cells capable of emulating the biological processes of living systems.
- Researchers develop 'founding document' on synthetic cell developmenton May 3, 2024 at 1:01 am
Cells are the fundamental units of life, forming the variety of all living things on Earth as individual cells and multicellular organisms. To better understand how cells perform the essential ...
- Biomea Fusion Reports First Quarter 2024 Financial Results and Corporate Highlightson May 2, 2024 at 9:05 am
Patients with type 2 diabetes have lost about 50% of their pool of beta cells while patients with type 1 diabetes ... A covalent small molecule is a synthetic compound that forms a permanent bond to ...
- What’s Next In The Ozempic Era?on April 25, 2024 at 12:30 pm
A new family of drugs is changing the way scientists are thinking about obesity — and more uses are on the horizon ...
- What’s the Difference Between AHAs and BHAs?on April 18, 2024 at 5:00 pm
Our expert staff answers frequently asked questions in their areas of expertise and defines common terms so you can be a smarter shopper. Read more here. AHAs and BHAs are common chemical ...
via Google News and Bing News