Goal is to Distinguish Between Viral and Bacterial Infections, Reduce Unnecessary Use of Antibiotics
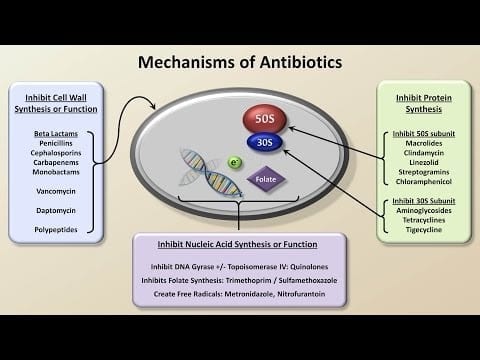
Antibiotics are lifesaving drugs, but overuse is leading to one of the world’s most pressing health threats: antibiotic resistance. Researchers at the University of Rochester Medical Center are developing a tool to help physicians prescribe antibiotics to patients who really need them, and avoid giving them to individuals who don’t.
Scientists from the University’s National Institutes of Health-funded Respiratory Pathogens Research Center identified 11 genetic markers in blood that accurately distinguished between viral and bacterial infections (antibiotics help us fight bacterial infections, but aren’t effective and shouldn’t be used to treat viruses). The finding, published in the journal Scientific Reports, is important because physicians don’t have a good way to confirm bacterial infections like pneumonia and more-often-than-not default to an antibiotic.
“It’s extremely difficult to interpret what’s causing a respiratory tract infection, especially in very ill patients who come to the hospital with a high fever, cough, shortness of breath and other concerning symptoms,” said Ann R. Falsey, M.D., lead study author, professor and interim chief of the Infectious Diseases Division at UR Medicine’s Strong Memorial Hospital. “My goal is to develop a tool that physicians can use to rule out a bacterial infection with enough certainty that they are comfortable, and their patients are comfortable, foregoing an antibiotic.”
Falsey’s project caught the attention of the federal government; she’s one of 10 semifinalists in the Antimicrobial Resistance Diagnostic Challenge, a competition sponsored by NIH and the Biomedical Advanced Research and Development Authority to help combat the development and spread of drug resistant bacteria. Selected from among 74 submissions, Falsey received $50,000 to continue her research and develop a prototype diagnostic test, such as a blood test, using the genetic markers her team identified.
A group of 94 adults hospitalized with lower respiratory tract infections were recruited to participate in Falsey’s study. The team gathered clinical data, took blood from each patient, and conducted a battery of microbiologic tests to determine which individuals had a bacterial infection (41 patients) and which had a non-bacterial or viral infection (53 patients). Thomas J. Mariani, Ph.D., professor of Pediatrics and Biomedical Genetics at URMC, used complex genetic and statistical analysis to pinpoint markers in the blood that correctly classified the patients with bacterial infections 80 to 90 percent of the time.
“Our genes react differently to a virus than they do to bacteria,” said Mariani, a member of the Respiratory Pathogens Research Center (RPRC). “Rather than trying to detect the specific organism that’s making an individual sick, we’re using genetic data to help us determine what’s affecting the patient and when an antibiotic is appropriate or not.”
Falsey, co-director of the RPRC, and Mariani say that the main limitation of their study is the small sample size and that the genetic classifiers selected from the study population may not prove to be universal to all patients
Learn more: URMC Researchers Developing New Tool to Fight Antibiotic Resistance
The Latest on: Antibiotic resistance
[google_news title=”” keyword=”antibiotic resistance” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]- Antibiotics use for acute sinusitis in children reduces treatment failures: Insights from meta-analysison May 12, 2024 at 8:29 pm
USA: Acute sinusitis is a common childhood ailment characterized by inflammation of the paranasal sinuses, often triggered by viral upper respiratory tract infections. While antibiotics have ...
- Warning of deadly drug-resistant disease on the rise across Dorseton May 12, 2024 at 8:22 pm
The Government has vowed to tackle the spread of a drug-resistant disease branded a "significant threat" to public health.
- In a new book, a scientist suggests ways to combat fast-spreading superbugs that defeat antibioticson May 12, 2024 at 5:00 pm
The story of antibiotics is a cautionary tale of a huge scientific triumph followed by great complacency. Today, antibiotic resistance is a silent, hidden pandemic, with profound consequences for ...
- ‘Diary of a Dying Girl’: A mother’s loss launches a global effort to fight antibiotic resistanceon May 12, 2024 at 10:30 am
Diane Shader Smith’s daughter, like thousands who die each year from drug-resistant infections, might have been saved if treatment came faster. Her mission now is to make sure it does.
- Warning over 'significant threat' drug-resistant disease on the rise in south Essexon May 12, 2024 at 4:26 am
The Government has vowed to tackle the spread of a drug-resistant disease branded a "significant threat" to public health.
- A mother’s loss launches a global effort to fight antibiotic resistanceon May 11, 2024 at 6:00 pm
Diary Of A Dying Girl” excerpts Mallory Smith's own writings, which chronicle her 13-year battle against an antibiotic-resistant lung infection.
- Tackling the hidden pandemic of antibiotic-resistant superbugson May 11, 2024 at 10:24 am
These superbugs then transfer some drug-defeating genes to other bacteria causing a pandemic of superbugs. It’s a vicious cycle. But water is not our only worry. Recent reports of the use of ...
- Stem cell treatments in Mexico linked to drug-resistant meningitis, joint infectionson May 9, 2024 at 12:35 pm
Antibiotic-resistant meningitis or severe, long-lasting joint infections: That's what three U.S. "medical tourists" brought home after seeking out unapproved stem cell treatments in Mexico, according ...
- A global effort to fight antibiotic resistanceon May 9, 2024 at 8:52 am
In November 2017, days after her daughter Mallory Smith died from a drug-resistant infection at the age of 25, Diane Shader Smith typed a password into Mallory’s laptop. Her daughter gave it to her ...
- Changes in pig farming in the 20th century spread antibiotic-resistant Salmonella around the world, finds studyon May 9, 2024 at 7:44 am
Historical changes in pig farming led to the global spread of Salmonella, resistant to antibiotics—a new international study led by researchers at the University of Warwick suggests.
via Google News and Bing News