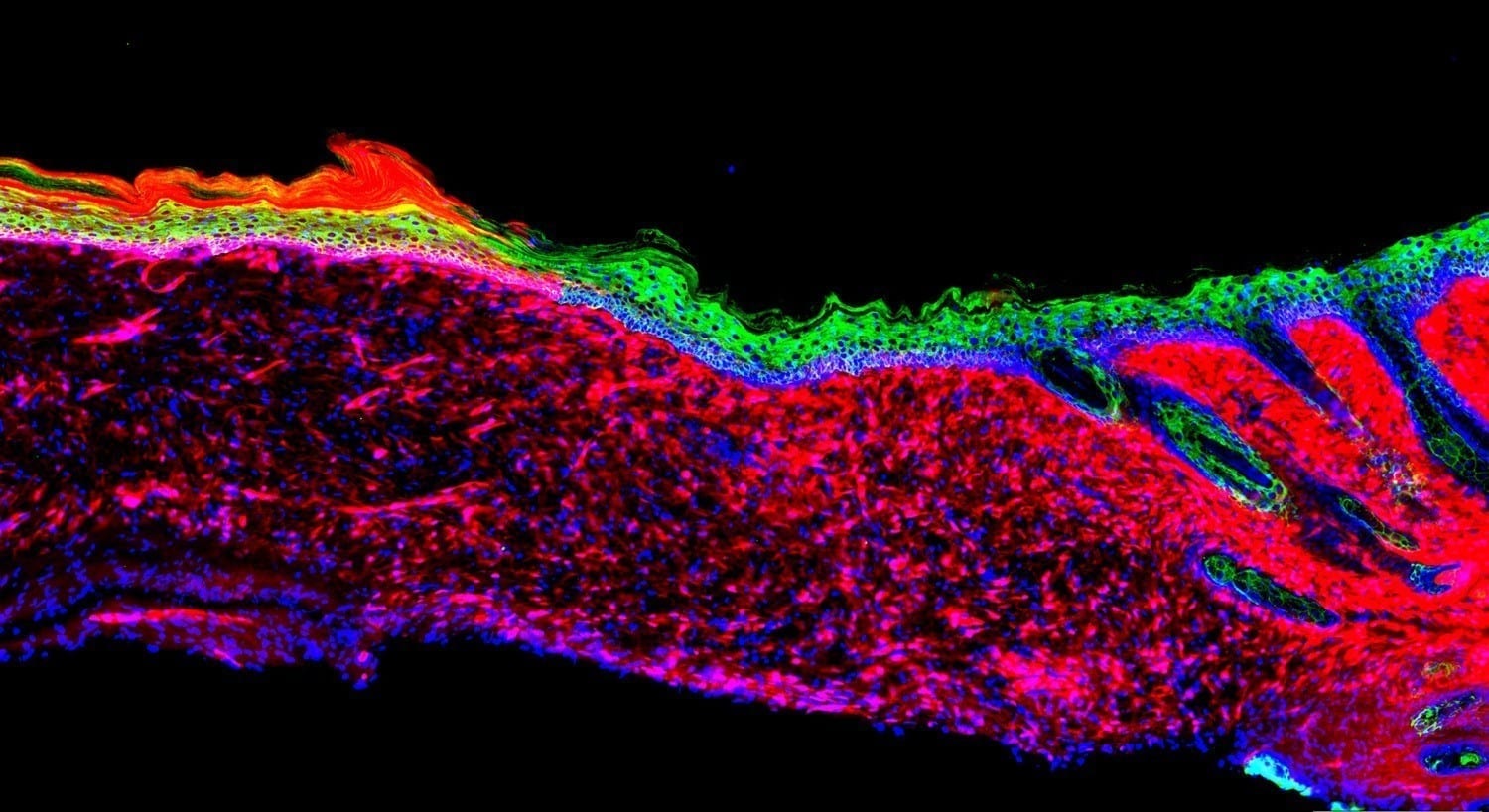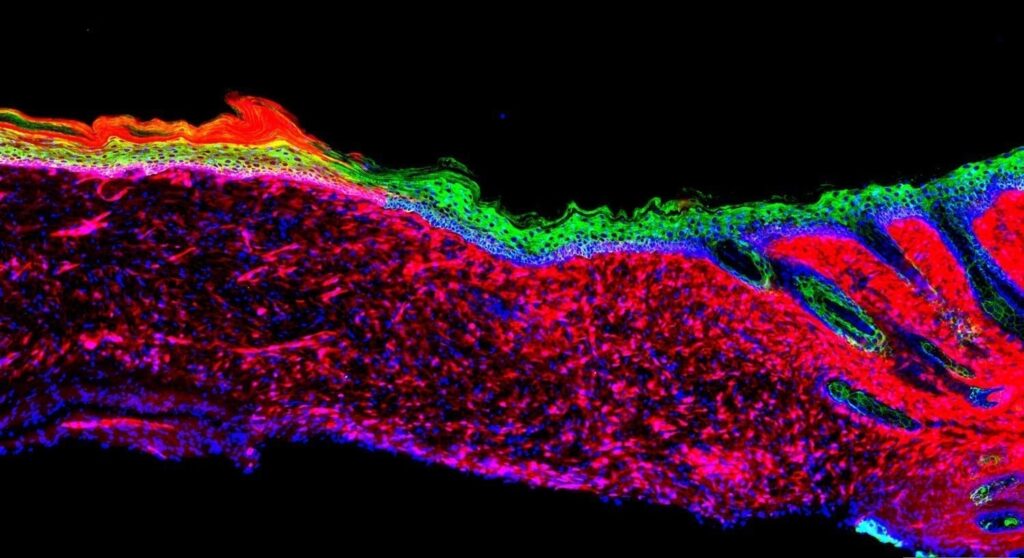
Credit: Salk Institute
Salk scientists develop new technique to heal large ulcers by reprogramming wound cells into skin cells
Plastic surgery to treat large cutaneous ulcers, including those seen in people with severe burns, bedsores or chronic diseases such as diabetes, may someday be a thing of the past. Scientists at the Salk Institute have developed a technique to directly convert the cells in an open wound into new skin cells. The approach relies on reprogramming the cells to a stem-cell-like state and could be useful for healing skin damage, countering the effects of aging and helping us to better understand skin cancer.
“Our observations constitute an initial proof of principle for in vivo regeneration of an entire three-dimensional tissue like the skin, not just individual cell types as previously shown,” says Salk Professor Juan Carlos Izpisua Belmonte, holder of the Roger Guillemin Chair and senior author of the new paper, published in the journal Nature on September 5, 2018. “This knowledge might not only be useful for enhancing skin repair but could also serve to guide in vivo regenerative strategies in other human pathological situations, as well as during aging, in which tissue repair is impaired.”
Cutaneous ulcers—wounds that can extend through multiple layers of the skin—are typically treated surgically, by transplanting existing skin to cover the wound. However, when the ulcer is especially large, it can be difficult for surgeons to graft enough skin. In these cases, researchers are able to isolate skin stem cells from a patient, grow them in the lab and transplant them back into the patient. However, such a procedure requires an extensive amount of time, which may put the patient’s life at risk and is sometimes not effective.
Izpisua Belmonte and Salk Research Associate Masakazu Kurita, who has a background in plastic surgery, knew that a critical step in wound recovery was the migration—or transplantation—of basal keratinocytes into wounds. These stem-cell-like cells act as precursors to the different types of skin cells. But large, severe wounds that have lost multiple layers of skin no longer have any basal keratinocytes. And even as these wounds heal, the cells multiplying in the area are mainly involved in wound closure and inflammation, rather than rebuilding healthy skin.
Izpisua Belmonte and Kurita wanted to directly convert these other cells into basal keratinocytes—without ever taking them out of the body. “We set out to make skin where there was no skin to start with,” says Kurita.
The researchers first compared the levels of different proteins of the two cell types (inflammation and keratinocytes) to get a sense of what they’d need to change to reprogram the cells’ identities. They pinpointed 55 “reprogramming factors” (proteins and RNA molecules) that were potentially involved in defining the distinct identity of the basal keratinocytes. Then, through trial and error and further experiments on each potential reprogramming factor, they narrowed the list down to four factors that could mediate the conversion to basal keratinocytes.
When the team topically treated skin ulcers on mice with the four factors, the ulcers grew healthy skin (known as epithelia) within 18 days. Over time, the epithelia expanded and connected to the surrounding skin, even in large ulcers. At three and six months later, the generated cells behaved like healthy skin cells in a number of molecular, genetic and cellular tests.
The researchers are planning more studies to optimize the technique and begin testing it in additional ulcer models.
“Before going to the clinic, we have to do more studies on the long-term safety of our approach and enhance the efficiency as much as possible,” says Kurita.
Learn more: The alchemy of healing: researchers turn open wounds into skin
The Latest on: Reprogramming cells
[google_news title=”” keyword=”reprogramming cells” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]
via Google News
The Latest on: Reprogramming cells
- Accessible Cell Therapies for Alzheimer's and Parkinson's Diseaseon April 25, 2024 at 10:21 pm
Researchers have now potentially advanced the accessible personalized cell-based therapies for Alzheimer's and Parkinson's diseases.
- New device improves stem cell generation and chance for accessible Alzheimer's cell therapyon April 24, 2024 at 12:11 pm
Researchers in Sweden say they have improved on a technique for converting regular skin cells into neural stem cells—an advance that they say helps close the gap for accessible personalized cell-based ...
- Scientists create artificial cells with capabilities for biomedical advancementson April 24, 2024 at 2:39 am
Researchers at the University of North Carolina , have successfully created artificial cells capable of mimicking natural cellular behaviour ...
- Self-assembling synthetic cells act like living cells with extra abilitieson April 23, 2024 at 5:00 pm
Blurring the line between artificial and living materials, these cells can be reprogrammed to perform multiple functions, opening the door to new synthetic biology tech that goes beyond nature’s ...
- Researchers develop a new way to safely boost immune cells to fight canceron April 22, 2024 at 11:48 am
Researchers explore a cancer immunotherapy treatment that involves activating the immune cells in the body and reprogramming them to attack and destroy cancer cells. This therapeutic method frequently ...
- Reprogramming the immune system to attack cancer cellson April 22, 2024 at 11:31 am
Researchers at Virginia Tech's developed a new therapy to target cancer with localized cytokine treatment to boost the immune system.
- Breakthrough in Bioinformatics: AI Predicts Cell Type Transformationson April 22, 2024 at 3:35 am
AI analyzes accessible data to pinpoint genetic modifications that alter cellular activity. Advances in gene sequencing technology and computing power have significantly increased the availability of ...
- Cancer Breakthrough Found to Boost Immune Cells Without Harmful Side-Effects By Directing Protein Cytokineson April 21, 2024 at 7:00 am
A new way to safely boost immune cells to fight cancer—avoiding harmful side-effects such as hair loss—has been developed.
- New research pinpoints key pathways in prostate cancer's vulnerability to ferroptosison April 17, 2024 at 7:36 pm
Review examines the role of ferroptosis, an iron-dependent form of cell death, in prostate cancer, exploring its underlying molecular mechanisms and potential for targeted therapeutic strategies.
- Reprogramming metastatic tumour cells with embryonic microenvironmentson April 14, 2024 at 5:00 pm
The embryonic neural crest microenvironment of the chick provides an attractive model system to explore melanoma tumour cell reprogramming. Human metastatic melanoma cells transplanted into the ...
via Bing News