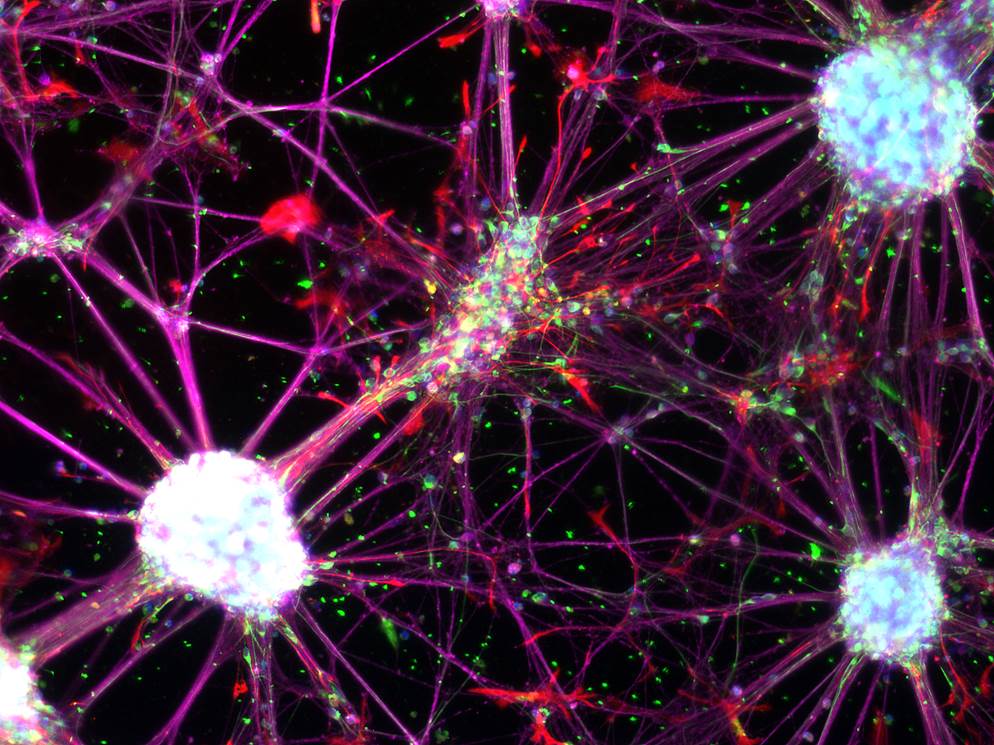
Scientists from the German Cancer Research Center (DKFZ) and the stem cell institute HI-STEM* in Heidelberg have succeeded for the first time in directly reprogramming human blood cells into a previously unknown type of neural stem cell.
These induced stem cells are similar to those that occur during the early embryonic development of the central nervous system. They can be modified and multiplied indefinitely in the culture dish and can represent an important basis for the development of regenerative therapies.
Stem cells are considered to be the all-rounders of our tissues: they can multiply indefinitely and then – if they are pluripotent embryonic stem cells – generate all conceivable cell types. In 2006, the Japanese scientist Shinya Yamanaka recognized that such cells could also be produced in the laboratory – from mature body cells. Four genetic factors alone are sufficient to reverse the course of development and produce so-called induced pluripotent stem cells (iPS) that have identical properties to embryonic stem cells. Yamanaka was awarded the Nobel Prize for Medicine in 2012 for this discovery.
“This was a major breakthrough for stem cell research,” said Andreas Trumpp, German Cancer Research Center (DKFZ) and Director of HI-STEM in Heidelberg. “This applies in particular to for research in Germany, where the generation of human embryonic stem cells is not permitted. Stem cells have enormous potential both for basic research and for the development of regenerative therapies that aim to restore diseased tissue in patients. However, reprogramming is also associated with problems: For example, pluripotent cells can form germ line tumors, so-called teratomas.
Another possibility is not to completely turn back the course of development. For the first time, Trumpp’s team has succeeded in reprogramming mature human cells in such a way that a defined type of induced neural stem cells is produced that can multiply almost indefinitely. “We used four genetic factors like Yamanaka, but different ones for our reprogramming,” explains Marc Christian Thier, first author of the study. “We assumed that our factors would allow reprogramming to an early stage of development of the nervous system.”
In the past, other research groups also reprogrammed connective tissue cells into mature nerve cells or neural precursor cells. However, these artificially produced nerve cells often could not be expanded and could therefore hardly be used for therapeutic purposes. “Often, it was a heterogeneous mixture of different cell types that might not exist in the body under physiological conditions,” said Andreas Trumpp explaining the problems.
Together with stem cell researcher Frank Edenhofer from the University of Innsbruck and neuroscientist Hannah Monyer from DKFZ and the Heidelberg University Hospital, Trumpp and his team have succeeded in reprogramming different human cells: connective tissue cells of the skin or pancreas as well as peripheral blood cells. “The origin of the cells had no influence on the properties of the stem cells,” said Thier. In particular, the possibility of extracting neural stem cells from the blood of patients without invasive intervention is a decisive advantage for future therapeutic approaches.
What is special about the reprogrammed cells of the Heidelberg researchers is that they are a homogeneous cell type that resembles a stage of neural stem cells that occurs during the embryonic development of the nervous system. “Corresponding cells exist in mice and probably also in humans during early embryonic brain development,” said Thier. “We have described here a new neural stem cell type in the mammalian embryo.
These so called “induced Neural Plate Border Stem Cells” (iNBSCs) have a broad development potential. The iNBSCs of the Heidelberg scientists are expandable and multipotent and can develop in two different directions. On the one hand, they can take the path of development to mature nerve cells and their supplier cells, the glial cells, i.e. become cells of the central nervous system. On the other hand, they can also develop into cells of the neural crest, from which different cell types emerge, for example peripheral sensitive nerve cells or cartilage and bones of the skull.
The iNBSCs thus form an ideal basis for generating a broad range of different cell types for an individual patient. “These cells have the same genetic material as the donor and are therefore presumably recognized as “self” by the immune system and are not rejected,” explains Thier.
The CRISPR/Cas9 gene scissors can be used to modify the iNBSC or repair genetic defects, as the scientists have shown in their experiments. “They are therefore of interesting both for basic research and the search for new active substances and for the development of regenerative therapies, for example in patients with diseases of the nervous system. However until we can use them in patients, a lot of research work will still be necessary,” emphasizes Trumpp.
The Latest on: Regenerative medicine
[google_news title=”” keyword=”regenerative medicine” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]
via Google News
The Latest on: Regenerative medicine
- New prototype that regenerates stem cells may repair IPF scarringon April 26, 2024 at 10:42 am
Researchers developed NZ-97, an inhalable drug that stimulates the growth of stem cells in the lungs, potentially repairing scarring in IPF.
- Regenerative Medicine Market Size Expected to Reach USD 154.05 Bn by 2033on April 26, 2024 at 8:10 am
The global regenerative medicine market size is expected to reach around USD 154.05 billion by 2033 increasing from USD 29.42 billion in 2023, growing at a healthy CAGR of 18% from 2024 to 2033.Ottawa ...
- ROSM can help reduce pain & enhance mobilityon April 26, 2024 at 2:00 am
Struggling with pain that limits your mobility? ROSM in the D.C., Maryland, and Virginia area offers advanced treatments to help you get back to daily activity!
- Hybrid brain lets one species' neurons help out another'son April 25, 2024 at 9:53 pm
Adding rat stem cells to a mouse embryo resulted in a ‘hybrid brain’ in which the rat cells stepped in to restore function when the mouse’s sense of smell was removed, new research has shown. It’s the ...
- Cabinet approves two bills on regenerative medicineon April 25, 2024 at 9:00 am
The draft regenerative medicine bill stipulates that only government-certified medical institutions can administer such treatments, with individuals or organizations that administer them without ...
- Is Telepathy Possible? Perhaps, Due To New Technologyon April 24, 2024 at 11:00 am
Telepathy is generally considered pure science fiction; fun, but never something that will actually happen. But new research suggests we may be closer than we think.
- What Is Drug Repurposing And Why Is It A Game-Changer In Regenerative Medicine?on April 23, 2024 at 7:55 am
Repurposed drugs have already undergone rigorous testing for safety and efficacy in other medical conditions. It enables researchers to fast-track their investigations, saving time and resources.
- How Regenerative Medicine Can prevent Autism Spectrum Disorder, Expert Explainson April 22, 2024 at 11:51 pm
Central to regenerative medicine's approach to treating autism is the rejuvenation of damaged neural networks. Stem cell therapies hold promise for replenishing depleted or dysfunctional neural ...
- Kansas Regenerative Medicine Center celebrates 10 years of transformative healthcareon April 18, 2024 at 11:29 am
Milestone achieved by Kansas Regenerative Medicine Center as the organizations marks 10 years of helping patients.
- Immunotherapy Regenerative Medicine Clinic on Using Stem Cells to Activate the Body's Natural Healing Poweron April 18, 2024 at 10:02 am
Stem cell therapy, a cornerstone of regenerative medicine, has shown immense potential in treating autoimmune diseases, aging conditions, and ...
via Bing News










