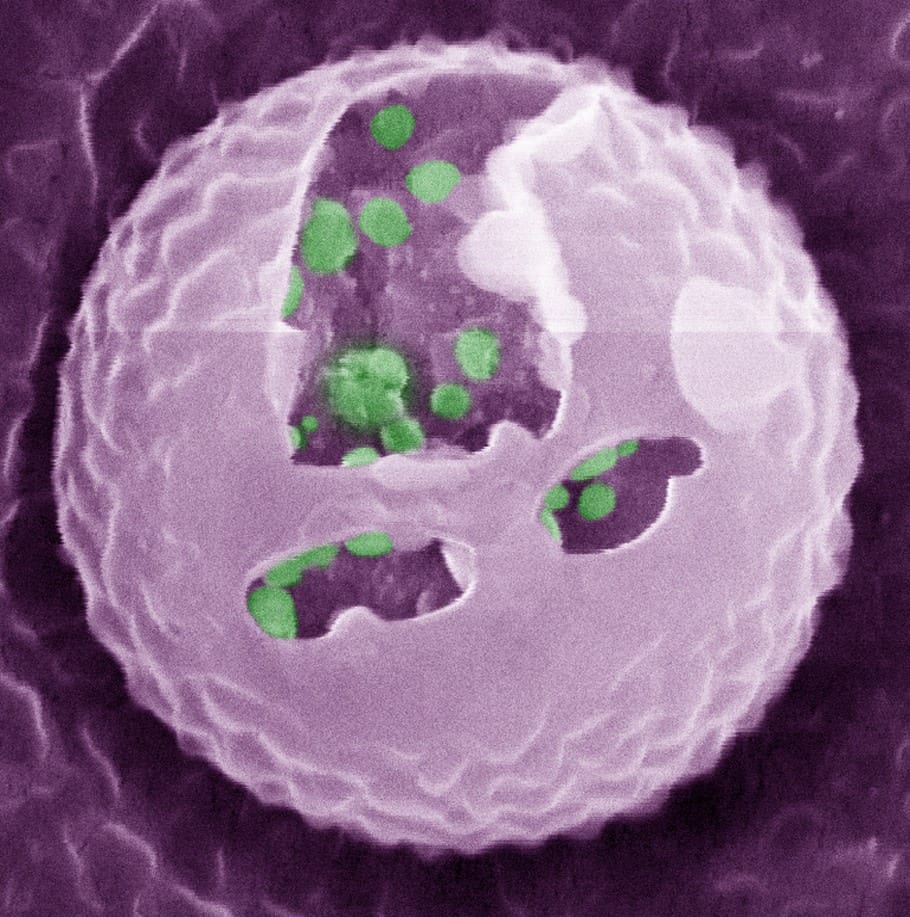
In lab experiments and animal models, UNC and NC State researchers led by Zhen Gu, PhD, designed synthetic beta cells to secrete insulin in response to high blood sugar.
Treating type 1 diabetes and some cases of type 2 diabetes has long required painful and frequent insulin injections or a mechanical insulin pump for insulin infusion. But researchers from the University of North Carolina and NC State have now developed what could be a much more patient-friendly option: artificial cells that automatically release insulin into the bloodstream when glucose levels rise.
These “artificial beta cells” (A?Cs) mimic the functions of the body’s natural glucose-controllers, the insulin-secreting beta cells of the pancreas. The loss or dysfunction of these cells causes type 1 diabetes and many cases of type 2 diabetes. The idea is that the A?Cs could be subcutaneously inserted into patients, which would be replaced every few days, or by a painless and disposable skin patch.
As the researchers report in Nature Chemical Biology, a single injection of the A?Cs into diabetic mice lacking beta cells quickly normalized the animals’ blood glucose levels and kept those levels normal for up to five days.
“Our plan now is to further optimize and test these synthetic cells in larger animals, develop a skin patch delivery system for them, and ultimately test them in people with diabetes,” said principal investigator Zhen Gu, PhD, a professor in the Joint UNC/NC State Department of Biomedical Engineering. Gu also holds appointments in the UNC School of Medicine, the UNC Eshelman School of Pharmacy, and the UNC Diabetes Care Center.
At least six million people in the United States use insulin as a diabetes treatment, either by injection or a mechanical pump. So far, delivered insulin in pill form has been challenging because it’s a large molecule that would be destroyed by digestive enzymes and acids before it could reach the bloodstream.
The major problem with current insulin treatments, however, is not that they can’t be delivered in a pill, but that they can’t control blood glucose levels automatically and efficiently, as normal insulin-secreting pancreatic cells do. Transplants of pancreatic cells can solve that problem in some cases. However, such cell transplants are expensive, require donor cells that are often in short supply, require immune-suppressing drugs, and often fail due to the destruction of the transplanted cells.

- False color Cryo-Scanning Electron Microscope image of the artificial beta cells. (Gu Lab, UNC-NC State)
Gu and colleagues have been researching solutions to the insulin-delivery problem for much of the past decade. For this project, they adopted a particularly ambitious approach: making artificial cells that, to a great extent, do what natural pancreatic beta cells do.
Gu’s A?Cs are constructed with a simplified version of a normal cell’s two-layered lipid membrane. The key innovation is what these cells contain: specially designed, insulin-stuffed vesicles. A rise in blood glucose levels leads to chemical changes in the vesicle coating, causing the vesicles to start fusing with the A?C’s outer membrane – thus releasing the insulin payloads.
“This is the first demonstration using such a vesicle fusion process for delivering insulin that employs insulin-containing vesicles like those found in a beta cell and can reproduce the beta cell’s functions in sensing glucose and responding with insulin ’secretion’,” said Zhaowei Chen, PhD, a lead author and postdoctoral researcher in Gu’s lab.
The A?Cs showed a rapid responsiveness to excess glucose levels in lab-dish tests and in diabetic mice without beta cells. “The mice went from hyperglycemic to normoglycemic within an hour, and they remained normoglycemic for up to five days after that,” Gu said. Control mice injected with no-insulin A?Cs remained hyperglycemic.
Gu and colleagues plan further preclinical tests and expect to develop a method for delivering the cells painlessly via a skin patch that could be simply replaced.
Co-author John Buse, MD, PhD, the Verne S. Caviness Distinguished Professor at UNC, chief of the division of endocrinology, and director of the UNC Diabetes Care Center, said, “There is still much work needed to optimize this artificial-cell approach before human studies are attempted, but these results so far are a remarkable, creative first step to a new way to solve the diabetes problem using chemical engineering as opposed to mechanical pumps or living transplants.”
Gu and his team are also working separately on a cell-free skin patch, a “smart insulin patch” that senses blood glucose levels and secretes insulin into the bloodstream as needed.
Learn more: Smart Artificial Beta Cells Could Lead to New Diabetes Treatment
The Latest on: Synthetic beta cells
[google_news title=”” keyword=”Synthetic beta cells” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]- Pathogenesis of Type 2 Diabeteson April 26, 2024 at 5:00 pm
The beta cells in genetically susceptible individuals become impaired, leading to delayed and insufficient insulin secretion. Due to decreasing beta-cell function, the individual with insulin ...
- What’s Next In The Ozempic Era?on April 25, 2024 at 12:30 pm
A new family of drugs is changing the way scientists are thinking about obesity — and more uses are on the horizon ...
- “Truly Amazing” – Quantum Dots Successfully Synthesized Inside Living Cells!on April 24, 2024 at 11:43 pm
A recent study published in the journal National Science Review demonstrates the synthesis of quantum dots (QDs) in the nucleus of live cells. The research was conducted by Dr. Hu Yusi, Associate ...
- Self-assembling synthetic cells act like living cells with extra abilitieson April 23, 2024 at 5:00 pm
Using DNA and proteins, scientists have created new synthetic cells that act like living cells. Blurring the line between artificial and living materials, these cells can be reprogrammed to perform ...
- Beta-Cell Differentiation From Nonendocrine Epithelial Cells of the Adult Human Pancreason April 22, 2024 at 4:59 pm
Nat Med. 2006;12(3):310-316. In conclusion, our study addresses an important fundamental question about beta-cell regeneration: namely, whether regeneration occurs by replication of preexisting ...
- Beyond biology: Creating dynamic synthetic cells with programmable DNAon April 22, 2024 at 4:59 pm
While living cells are more complex than the synthetic ones created by the Freeman Lab, they are also more unpredictable and more susceptible to hostile environments, like severe temperatures. "The ...
- AI tool creates 'synthetic' images of cells for enhanced microscopy analysison April 22, 2024 at 1:48 pm
Observing individual cells through microscopes can reveal a range of important cell biological phenomena that frequently play a role in human diseases, but the process of distinguishing single cells ...
- The 20 Best Skincare Brands in 2024on April 22, 2024 at 12:10 pm
Branded content. Us Weekly has affiliate partnerships so we may receive compensation for some links to products and services. Whether you are a skincare aficionado or are just learning the ropes, you ...
- Hitchhiking of synthetic antigen stimulates antibody production against cancer cellson April 22, 2024 at 8:04 am
Researchers at the Indian Institute of Science (IISc) have designed a synthetic compound (antigen) that can latch on to a protein in blood and hitchhike a ride to the lymph node, where it can boost ...
- What’s the Difference Between AHAs and BHAs?on April 19, 2024 at 12:09 pm
Instead, AHAs do their work superficially on the top layers of the skin. When applied to the skin, they loosen the bonds between dead skin cells so that they’re replaced with new ones. These acids are ...
via Google News and Bing News










