Technion researchers have successfully established a new approach for pacing the heart and synchronizing its mechanical activity without the use of a conventional electrical pacemaker. This novel biologic strategy employs light-sensitive genes that can be injected into the heart and then activated by flashes of blue light.
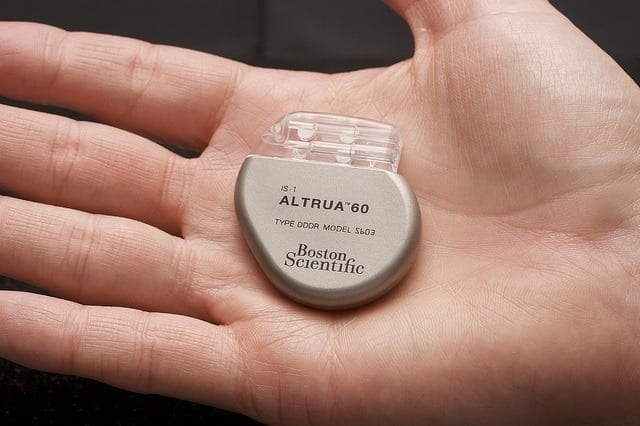
More than 3 million people worldwide have had electronic pacemakers implanted. The most common indication for a pacemaker is the treatment of a slow heart beat which can put patients at risk for fainting, heart failure, and even death. Pacemakers work by sending electrical signals to the heart to regulate the heart beat. Pacemakers can also be used for cardiac resynchronization therapy (CRT), an approach aiming to synchronize the contraction of the heart’s two ventricles in order to improve heart function, symptom status and decrease mortality in some patients who suffer from heart failure.
The new optogenetic approach for cardiac pacing and resynchronization was developed by Prof. Lior Gepstein and Dr. Udi Nussinovitch of the Technion-Israel Institute of Technology’s Rappaport Faculty of Medicine, and Rambam Medical Center.
“Our work is the first to suggest a non-electrical approach to cardiac resynchronization therapy,” Gepstein said. “Before this, there have been a number of elegant gene therapy and cell therapy approaches for generating biological pacemakers that can pace the heart from a single spot. However it was impossible to use such approaches to activate the heart simultaneously from a number of sites for resynchronization therapy.”
If the biological pacemaker can be adapted for humans, it could help patients avoid many of the drawbacks of electrical pacemakers. These include the surgical procedure needed to implant the device, the risk of infection, the limitation on the number and locations of the pacing wires used, the possible decline in cardiac function resulting from the change in the normal electrical activation pattern, and the limitations on implantation in children.
“This is a very important proof-of-concept experiment, which for the first time, demonstrates a mechanism to pace the heart without the need for wires and allows for simultaneous pacing from multiple sites,” said Dr. Jeffrey Olgin, chief of the Division of Cardiology and co-director of the Heart and Vascular Center at the University of California, San Francisco. “The most common site of failure of current pacemakers are the leads or wires that connect the heart muscle to the electrical impulse. The approach demonstrated in this paper has the potential to eliminate these wires or have a single lead excite multiple sites simultaneously.”
Pacing the heart with light is part of the emerging field of optogenetics, which has gained considerable momentum in the field of brain research. Researchers working in the field have been taking light-sensitive genes from algae and placing them in cells where they act like a switch, turning certain behaviors on or off when the cells are exposed to pulses of light.
As they report in the journal Nature Biotechnology, the Technion researchers injected one of these algae genes (channelorhodopsin-2) into a specific area of rat heart muscle. The scientists then showed that the light-sensitive protein expressed at this site could be turned on with flashes of blue light and drive the heart muscle to contract. By altering the frequency of the flashes, Gepstein and Nussinovitch could control and regulate the heart rate. They went on to deliver the gene to several places in the heart’s pumping chambers, and demonstrated the ability to simultaneously activate the heart muscle from many places in an effort to synchronize the heart’s pumping function.
Scientists will need to do more research for this optogenetic-based pacemaker strategy to become a reality in human health, Gepstein said. For instance, the gene injected in the rat experiments is sensitive to blue light which has poor tissue penetration potentially limiting its utility in large animals or humans.
“This means that the affected cells have to be relatively superficial–near the surface of the heart–and that an optical fiber should be implanted bringing the illumination beam as close as possible to the cells,” Gepstein said. “A potential solution in the future may be the development of similar light-sensitive proteins that will be responsive to light in the near-red or even infra-red spectrum, which penetrates tissue much better, allowing illumination from a long distance.”
Read more: BLUE LIGHT SETS THE BEAT IN BIOLOGICAL PACEMAKER
The Latest on: Biological Pacemaker
[google_news title=”” keyword=”Biological Pacemaker” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]
via Google News
The Latest on: Biological Pacemaker
- Beware What You Wear With Your Pacemaker or ICDon April 25, 2024 at 5:00 pm
Relatively weak magnets in consumer products have always posed some risk, usually very low, to the function of pacemakers and implantable cardioverter-defibrillators (ICDs). However, stronger ...
- The relationship between calcium consumption at various times of the day and cardiovascular diseaseon April 24, 2024 at 12:13 am
However, the relationship between calcium consumption at various times of the day and cardiovascular disease is unclear. The present study examined the relationship between dietary calcium consumption ...
- Permanent Pacemaker Implantation Following Cardiac Surgery: Indications and Long-Term Follow-Upon April 23, 2024 at 5:00 pm
Background: Conduction disturbances requiring permanent pacemaker implantation after heart surgery occur in about 1.5% of patients. Early pacemaker implantation may reduce morbidity and ...
- Identity Pacemaker from St. Jude Medicalon April 23, 2024 at 5:00 pm
The Identity pacemaker models 5370 and 5376 feature AF management, a suite of therapeutic and diagnostic capabilities designed to manage pacemaker patients suffering from AF. This tool kit includes: ...
- Mechanical engineers develop miniaturized, hydrogel-based electric generators for biomedical deviceson April 22, 2024 at 6:05 am
Mechanoelectrical energy conversion offers a promising solution for powering miniaturized biomedical devices, such as cardiac pacemakers, brain stimulators, wearable drug delivery systems, and more.
- Your body has an internal clock that dictates when you eat, sleep and might have a heart attack – all based on time of dayon April 6, 2024 at 5:00 pm
Anyone who has suffered from jet lag or struggled after turning the clock forward or back an hour for daylight saving time knows all about what researchers call your biological clock, or circadian ...
- Neurons and networks in daily rhythmson April 1, 2024 at 5:00 pm
The nervous system is never silent, and neurons often show daily rhythms in their gene and electrical activities. These rhythms arise from near 24-hour feedback loops that involve identified genes ...
- Arnold Schwarzenegger Shares Photo Wearing Pacemaker, Says It Won't Conflict with FUBAR Season 2on March 28, 2024 at 7:57 pm
The actor shared this week that he recently underwent surgery to have the pacemaker implanted Arnold Schwarzenegger/Instagram Arnold Schwarzenegger is in good spirits as he recovers from getting a ...
- Arnold Schwarzenegger Shares Pacemaker Health Update, Says He’ll ‘Be Ready’ to Shoot ‘Fubar’ Next Monthon March 28, 2024 at 6:34 pm
Arnold Schwarzenegger is giving his fans a health update. Three days after revealing he had surgery to implant a pacemaker, Schwarzenegger shared that he was in good health and will “be ready ...
- The Terminator Gets a Pacemaker — What That Meanson March 28, 2024 at 5:00 pm
Actor Arnold Schwarzenegger revealed he had a pacemaker installed to treat an irregular heartbeat. He was born with a bicuspid aortic heart valve, which can make the heart work much harder than it ...
via Bing News