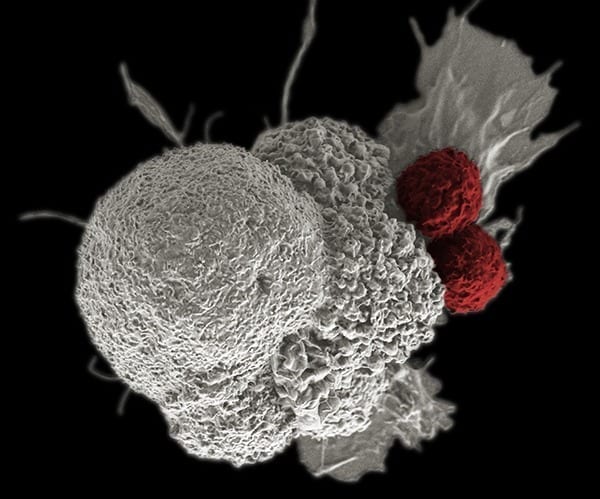
Tumor-infiltrating lymphocytes go after tumors by recognizing and then directly attacking each cell with a poisonous spray.
Novel technology platform could bring individualized cell therapies to patients
Northwestern University researchers have developed a new tool to harness immune cells from tumors to fight cancer rapidly and effectively.
Their findings, published January 27 in the journal Nature Biomedical Engineering, showed a dramatic shrinkage in tumors in mice compared to traditional cell therapy methods. With a novel microfluidic device that could be 3D printed, the team multiplied, sorted through and harvested hundreds of millions of cells, recovering 400 percent more of the tumor-eating cells than current approaches.
Most treatments for cancer involve toxic chemicals and foreign substances, which cause harmful side effects and weaken the body’s immune response. Using tissue from one’s own body can eliminate side effects and risk of rejection, and many disease therapies in regenerative medicine and cancer treatment have gained traction in the clinic. But sometimes the wheels skid.
“People have been cured in the clinic of advanced melanoma through treatment with their own immune cells that were harvested out of tumor tissue,” said Shana O. Kelley, a pioneer in translational biotechnology and corresponding author on the paper. “The problem is, because of the way the cells are harvested, it only works in a very small number of patients.”
Kelley is the Neena B. Shwartz Professor of Chemistry and Biomedical Engineering at the Northwestern University Weinberg College of Arts and Sciences and Northwestern Engineering, and a professor of biochemistry and molecular genetics at Northwestern University Feinberg School of Medicine.
The cells of interest, called tumor-infiltrating lymphocytes (TILs), are natural immune cells that invade tumor tissue by engaging cells in a form of hand-to-hand combat that looks like someone using insecticide on a weed. But, in this scenario, previous researchers have been attacking the weeds with a half-expired cannister of chemicals.
This is the case in cell therapies used in clinics today, where a mixture of “exhausted” and “naïve” cells is used to treat tumors. After they are extracted from tissue, cells are grown in labs far away from the patients they were harvested from. By the time they’ve multiplied and are ready to be placed back in the body, many of the cells are exhausted and unable to fight, having been in the tumor for too long.
Assembling the best fighters
Using a new technology called microfluidic affinity targeting of infiltrating cells (MATIC), researchers can pinpoint which cells are most active through cell sorting techniques enabled with nanotechnology. In the paper, scientists used MATIC to find what the authors called the “Goldilocks population” of cells, producing dramatic results for the mice population they were looking at. Tumors in mice shrank dramatically — and in some mice disappeared completely — producing a large improvement in survival rates compared to more traditional methods of TIL recovery.
“Instead of giving mice this mixture of cells with different phenotypes, we’re giving them the one cell phenotype that can actually help them,” Kelley said. “You see much more potency and a much higher response rate when you really home in on the sweet spot of T cell reactivity.”
Reproducible, accessible technology
Because her team’s technology is small and easily reproducible, Kelley said it would be feasible to bring the 3D-printed device into hospital settings, rather than confining it to a lab. Getting cell therapy closer to patients would dramatically reduce research and development costs and ultimately deliver the treatment to more people.
Kelley joined Northwestern in August from the University of Toronto and has continued to study how her platform might advance cancer treatments. Now, she’s using the device to search for the same types of TILs in blood samples, which would eliminate the need for surgery to remove a small piece of tumor prior to this form of treatment.
When we take on the development of a new technology, we typically end up with a hammer, and then need to go find a nail. We got introduced to problems in cell therapy, and it was immediately apparent that this was a perfect fit.Neena B. Shwartz Professor of Chemistry and Biomedical Engineering
Kelley has launched a small company to commercialize her devices and plans to work with industry partners and collaborators at Northwestern to continue expanding use cases for the tool.
The platform itself has been used across applications, mostly for the analysis and measurement of rare cells in the body.
“When we take on the development of a new technology, we typically end up with a hammer, and then need to go find a nail,” Kelley said. “We got introduced to problems in cell therapy, and it was immediately apparent that this was a perfect fit.”
Neena B. Shwartz Professor of Chemistry and Biomedical Engineering
The first author of the study, PhD student Daniel Wang, is also joining Northwestern from the University of Toronto as a postdoctoral fellow and plans to continue developing new solutions for cell therapy in the Kelley group’s labs on the Chicago campus.
Original Article: Tumors Dramatically Shrink with New Approach to Cell Therapy
More from: Northwestern University | Northwestern University Feinberg School of Medicine
The Latest Updates from Bing News & Google News
Go deeper with Bing News on:
Microfluidic affinity targeting of infiltrating cells
- Nanoparticle researchers develop microfluidic platform for better delivery of gene therapy for lung disease
Drug delivery researchers at Oregon State University have developed a device with the potential to improve gene therapy for patients with inherited lung diseases such as cystic fibrosis.
- Study provides a blueprint of tumor-infiltrating B cells with therapeutic implications
In a study published in Science on May 3, researchers unveiled two responding patterns of tumor-infiltrating B cells with therapeutic implications.
- Antibody and Cell Therapy Development: The Life of Single Cells on Beacon® Platform
The Beacon platform provides a complete picture of single cell function through real-time imaging and multi-modal analysis on the same live single cell, with high throughput. Explore its advanced ...
- Researchers explore new cell target for cystic fibrosis treatment
Because some potential treatments of CF involve targeting and modifying the CFTR function at the genetic level in sick airway cells, the specific role various types of cells play in CF disease ...
- CAR T cell therapy targeting HER2 antigen shows promise against advanced sarcoma in phase I trial
The therapy uses chimeric antigen receptor (CAR) T cells engineered to target the HER2 protein, which is overexpressed on the surface of sarcoma cells. The HEROS 2.0 trial showed that this ...
Go deeper with Google Headlines on:
Microfluidic affinity targeting of infiltrating cells
[google_news title=”” keyword=”microfluidic affinity targeting of infiltrating cells” num_posts=”5″ blurb_length=”0″ show_thumb=”left”]
Go deeper with Bing News on:
Cell therapy
- UK toddler born deaf has hearing restored thanks to gene therapy treatment
Amazing science news this week comes from the UK, where a 1 year old baby who was born deaf due to a genetic condition called auditory neuropathy was treated with gene therapy.
- FDA’s Marks: Global Regulatory Convergence Vital to Cell & Gene Therapy Oversight
ASGCT 2024 session, CBER Director Peter Marks made the case for a better, “more convergent” global framework on cell and gene therapies, especially for rare diseases.
- Lisata’s Autologous T Cell Therapy Is Safe but Fails to Slow T1D Disease Progression, Trial Finds
An autologous and personalized regulatory T cell therapy is safe in patients with type 1 diabetes, but does not help preserve β-cell function.
- As Ozzy Osbourne announces stem cell therapy, experts urge caution, highlight risks
As rock legend Ozzy Osbourne has turned to stem cell therapy, some experts caution that the treatment is not for everyone. A doctor weighed in on the potential risks.
- Regeneron's cell medicines chief is crafting a new cell therapy 'secret sauce'
Phil Gregory’s new gig looks a whole lot like his old gig. It’s just that, under the umbrella of Regeneron, things have gotten a bit bigger. | Phil Gregory’s new gig looks a whole lot like his old gig ...
Go deeper with Google Headlines on:
Cell therapy
[google_news title=”” keyword=”cell therapy” num_posts=”5″ blurb_length=”0″ show_thumb=”left”]