New methods developed for the study could be applied to devise personalized, cell-based immunotherapies for epithelial ovarian cancer or other types of tumors
A Ludwig Cancer Research study shows that ovarian cancer, which has proved resistant to currently available immunotherapies, could be susceptible to personalized immunotherapy. Led by Ludwig Lausanne investigator Alexandre Harari and George Coukos, director of the Ludwig Institute for Cancer Research, Lausanne, the study shows that ovarian tumors harbor highly reactive killer T cells—which kill infected and cancerous cells—and demonstrates how they can be identified and selectively grown for use in personalized, cell-based immunotherapies.
“Tumors whose cells tend to be highly mutated, like those of melanoma and lung cancer, are the ones that respond best to immunotherapies,” says Harari. “It has long been a question whether we’d even be able to detect sufficiently mutation-reactive T cells in patients with tumors that have low mutational loads.”
Harari, Coukos and their colleagues report in Nature Communicationsthat, despite their low mutational load, epithelial ovarian tumors are infiltrated with T cells that are especially good at recognizing and killing cancer cells.
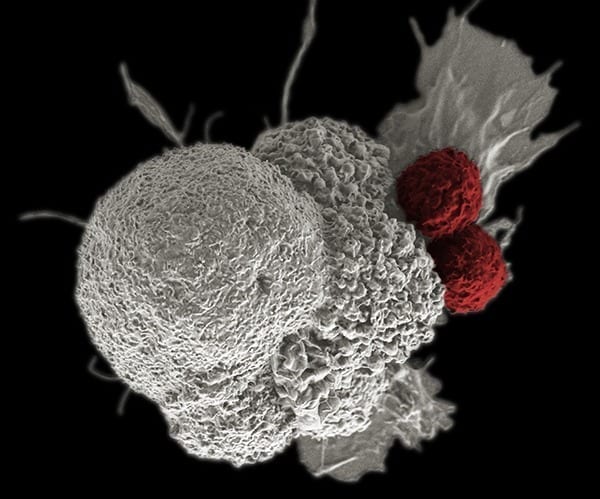
Cancer cells that have a relatively large number of mutations in their DNA express aberrant proteins—or neoantigens—that reveal the cancer to the immune system. Killer T cells recognize tiny, mutated bits of these antigens, known as neoepitopes. But neoepitopes vary wildly from patient to patient, even within the same type of cancer. This has long stymied efforts to develop generally effective therapies that target cancer antigens.
To get around this problem, researchers have been developing sophisticated methods to extract T cells from patients, select and expand those that best target a patient’s cancer and reinfuse them into the patient. These approaches usually rely on T cells extracted from the bloodstream, not those already inside the tumor, which are referred to as TILs (for tumor infiltrating lymphocytes).
Experimental therapies using T cells taken from the blood stream have not, however, worked very well against solid tumors. Further, when TILs have been used for such purposes, the proportion of what Harari calls the “juiciest” T cells—those recognizing mutations on cancer cells—tends to decline significantly when the cells are expanded in culture.
“To circumvent these problems, we developed a new methodology to identify highly reactive TILs and expand them in a manner that, rather than diluting the juiciest TILs, enriches them instead,” says Harari. “This allowed us to compare the activity of TILs that target neoepitopes with their counterparts in the peripheral bloodstream.”
The researchers show that killer T cells isolated from ovarian tumors using their method are much better at both recognizing neoepitopes than are those isolated from blood.
“We could even compare T cells from the two compartments targeting the exact same mutation and show that the TILs were more functional than the T cells we collected from the peripheral bloodstream,” says Harari.
Notably, the researchers found that, using their methods, highly reactive TILs could be obtained from some 90% of the ovarian cancer patients whose tumor samples they examined.
“The big message,” says Coukos, “is that future cell-based therapies can be envisioned for low mutational load tumors and should prioritize the use of TILs over T cells collected from peripheral blood. This novel strategy to obtain enriched TILs also offers great therapeutic opportunities.”
Harari, Coukos and their colleagues will now be applying their findings to an ambitious program to develop and streamline personalized immunotherapies for cancer patients currently underway at the Lausanne Branch of the Ludwig Institute for Cancer Research.
Learn more: LUDWIG STUDY EXTENDS THE POTENTIAL FOR PERSONALIZED IMMUNOTHERAPY TO A LARGE VARIETY OF CANCERS
The Latest on: Personalized cell-based immunotherapies
[google_news title=”” keyword=”personalized cell-based immunotherapies” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]
via Google News
The Latest on: Personalized cell-based immunotherapies
- Washington University in St. Louis Receives $5 Million Grant to Advance Innovative Immunotherapies Targeting Blood Cancerson May 10, 2024 at 5:38 pm
Researchers at Washington University School of Medicine in St. Louis have received a $5 million grant from the Leukemia & Lymphoma Society (LLS) to support research aimed at developing new immunothera ...
- How personalized medicine is transforming your health careon May 10, 2024 at 1:42 am
Motor neurons (white) and a blood vessel (red), derived from the ALS patient’s stem cells ... for Personalized Cancer Therapy. “You pick the right drugs for each patient based on the tumor ...
- AI predicts tumor-killing cells with high accuracyon May 7, 2024 at 4:23 pm
Using artificial intelligence, scientists have developed a powerful predictive model for identifying the most potent cancer killing immune cells for use in cancer immunotherapies.
- Glioblastoma vaccine turns brain tumors from cold to hot in humans and dogson May 7, 2024 at 2:29 am
A personalized mRNA-based cancer vaccine for glioblastoma with an “onion-like” delivery mechanism can prolong survival both in dogs and humans, the results of a small study have suggested.
- New approach for developing cancer vaccines could make immunotherapies more effective in acute myeloid leukemiaon May 3, 2024 at 12:13 pm
Acute myeloid leukemia (AML) is a type of blood cancer that forms in the soft marrow of the bones, typically attacking cells that would otherwise form the key component of the body's immunodefense ...
- MRNA vaccine effective in treating glioblastoma brain cancer in small trialon May 2, 2024 at 9:24 am
An experimental cancer vaccine can quickly reprogram a person's immune system to attack glioblastoma, the most aggressive and lethal form of brain cancer, a small, preliminary study has found.
- Understanding the 3D Cell Culture Revolutionon April 16, 2024 at 5:01 pm
“3D cell culture is taking cells out of that 2D environment ... Emerging organoid-immune co-culture models for cancer research: from oncoimmunology to personalized immunotherapies. J Immunother Cancer ...
- AACR 2024: Geneos Therapeutics’ Vaccine Outperforms Liver Cancer Immunotherapieson April 8, 2024 at 5:00 pm
Sardesai is doing this at Geneos, a clinical-stage biotherapeutics company focused on developing DNA-based personalized ... and without T cells, immunotherapies do not work. Even if the PTCV ...
- Researchers develop AI-based tool paving the way for personalized cancer treatmentson March 29, 2024 at 8:21 am
The work was published in the journal of Cell Systems ... Next-generation immunotherapies will be highly precise and tailored based on an individual's MHC molecules." The researchers envision ...
via Bing News