During infection or tumor growth, a type of specialized white blood cells called CD8+ T cells rapidly multiply within the spleen and lymph nodes and acquire the ability to kill diseased cells. Some of these killer T cells then migrate where required to vanquish the germs or cancers.
But how do killer T cells “learn” to leave their home base and amass within specific tissues like the skin, gut, and lung, or solid tumors? Finding the factors that cause T cells to function beyond the lymphoid system and in sites of infection or cancer has proven a tough challenge, but it’s essential for developing cancer-fighting immunotherapy strategies.
Writing in the journal Nature, researchers from The Scripps Research Institute and the University of California, San Diego report the discovery that a protein called “Runx3” programs killer T cells to establish residence in tumors and infection sites.
“Runx3 works on chromosomes inside killer T cells to program genes in way that enables the T cells to accumulate in a solid tumor,” said Matthew Pipkin, Ph.D., associate professor in the Department of Immunology and Microbiology on the Florida campus of The Scripps Research Institute.
The paper, “Runx3 programs CD8+ T cell residency in non-lymphoid tissues and tumors,” appears in Nature’s Dec. 14 issue.
There are two main strategies in cancer immunotherapy that employ killer T cells, Pipkin said. Checkpoint inhibitor blockade unleashes killer T cells, prompting them to accumulate in tumors more aggressively. Adoptive cell transfer, meanwhile, involves re-infusing a patient’s own immune cells after they have been engineered in the lab to recognize and destroy the patient’s specific cancer.
The adoptive cell transfer strategy has worked stunningly well in some blood cancers associated with the lymphoid system, so far. But there appears to be less efficient activity of T cells in solid tumors, Pipkin said.
“The gene programs and signals for how the T cells take up residence in tissues outside of the general circulation was not really well understood,” Pipkin said.
To discover factors that control T cell residency beyond the lymphoid system, Pipkin’s team worked collaboratively with the laboratory of UC San Diego’s Ananda Goldrath, who compared the gene expression of CD8+ T cells found in non-lymphoid tissue to those found in the general circulation. From a list of potential factors, they employed an RNA interference screening strategy which can test the actual function of thousands of factors simultaneously. Pipkin’s lab had developed the screening strategy in collaboration with Shane Crotty at the La Jolla Institute for Allergy and Immunology.
“We found a distinct pattern,” Pipkin said. “The screens showed that Runx3 is one at the top of a list of regulators essential for T cells to reside in nonlymphoid tissues.” Moreover, Runx3 was able to engage a specific gene program that is found in natural tissue-resident and tumor infiltrating CD8+ T cells, he said.
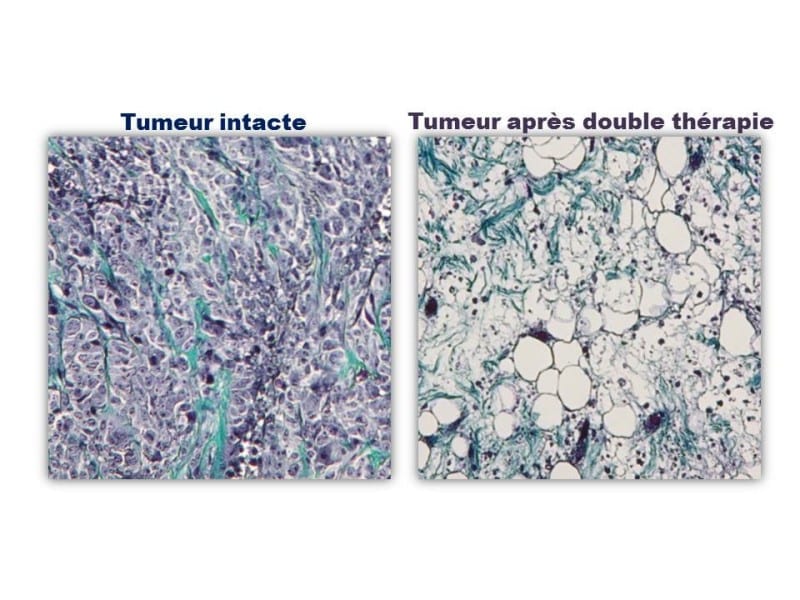
The group further assessed whether Runx3 had a role in directing white blood cells that attack solid tumors in mouse melanoma models. They found that adoptive cell transfer of cancer-specific killer T cells that overexpressed Runx3 delayed tumor growth and prolonged survival, while mouse models treated with those lacking Runx3 fared much worse than normal.
“If we enhance Runx3 activity in the cells, the tumors are significantly smaller and there is greater survival compared to the control group,” Pipkin said.
Knowing that modulating Runx3 activity in T cells influences their ability to reside in solid tumors opens new opportunities for improving cancer immunotherapy, Pipkin said.
“The upshot is we could probably use Runx3 to reprogram adoptively transferred cells to help drive them to amass in solid tumors,” he said. He added that a collaboration of specialists energized the research. “It was a fantastic collaboration, it all came together very quickly,” Pipkin said.
Learn more: Scientists discover possible master switch for programming cancer immunotherapy
The Latest on: Cancer immunotherapy
[google_news title=”” keyword=”cancer immunotherapy” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]- Gut bacteria enhance cancer immunotherapy in mouse studyon May 17, 2024 at 11:00 am
Roughly one in five cancer patients benefit from immunotherapy—a treatment that harnesses the immune system to fight cancer. Such an approach to beating cancer has seen significant success in lung ...
- Research finds the protein VISTA directly blocks T cells from functioning in immunotherapyon May 17, 2024 at 11:00 am
A Cleveland Clinic-led team of scientists and physicians have discovered that the immune checkpoint protein VISTA can directly turn off tumor-fighting T-cells during immunotherapy and resist treatment ...
- US FDA approves Amgen drug for small cell lung canceron May 17, 2024 at 10:56 am
The U.S. Food and Drug Administration on Thursday granted accelerated approval to Amgen's tarlatamab, a targeted immunotherapy for treating adults with advanced small cell lung cancer that has ...
- CU, GPO jointly develop cancer immunotherapy drugson May 17, 2024 at 10:26 am
Chulalongkorn University’s Faculty of Medicine announced a partnership with the Government Pharmaceutical Organization (GPO) to accelerate the development of antibody immunotherapy drugs for cancer ...
- Most cancer treatments are useless for patients with advanced tumors near end of lifeon May 17, 2024 at 8:27 am
Cutting-edge cancer treatments are essentially useless for patients barely clinging to life, a new study shows.
- Unlocking the body’s defences: understanding immunotherapyon May 16, 2024 at 10:27 am
Until now, chemo and radiation therapy have been main cancer treatments but they can also damage healthy tissues. Immunotherapy uses the body’s immune system to fight cancer with minimal harm ...
- Immunotherapy may boost survival after lung cancer surgeryon May 16, 2024 at 9:19 am
Immunotherapy can boost the survival of early-stage lung cancer patients eligible for surgery when it's combined with chemotherapy, a new clinical trial reports.
- New cancer research enables better immunotherapy treatmenton May 15, 2024 at 5:00 pm
As a result, they will be able to offer cancer patients more effective immunotherapy treatment. “Cancer cells have the ability to manipulate immune cells, evading the body’s natural defenses. By ...
- Pre- and post-surgical immunotherapy improves outcomes for patients with operable lung cancer, Phase III study findson May 15, 2024 at 2:00 pm
Compared with pre-surgical (neoadjuvant) chemotherapy alone, adding perioperative immunotherapy—given before and after surgery—significantly improved event-free survival (EFS) in patients with ...
- This time, it's personal: Enhancing patient response to cancer immunotherapyon May 15, 2024 at 12:12 pm
Immunotherapy has revolutionized the way we treat cancer in recent years. Instead of targeting the tumor itself, immunotherapies work by directing patients' immune systems to attack their tumors more ...
via Google News and Bing News