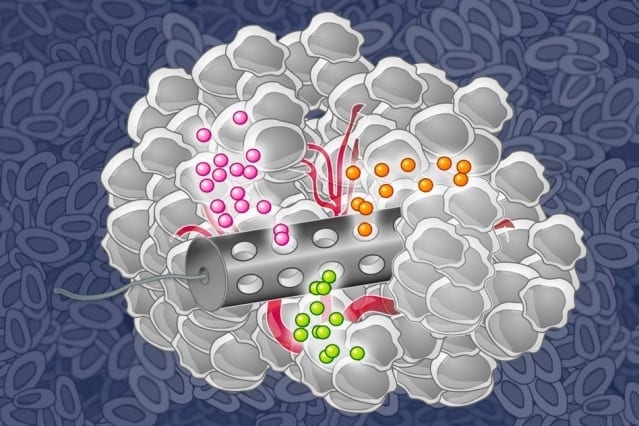
Image: Eric Smith (edited by Jose-Luis Olivares/MIT)
Implantable device could allow doctors to test cancer drugs in patients before prescribing chemotherapy
More than 100 drugs have been approved to treat cancer, but predicting which ones will help a particular patient is an inexact science at best.
A new device developed at MIT may change that. The implantable device, about the size of the grain of rice, can carry small doses of up to 30 different drugs. After implanting it in a tumor and letting the drugs diffuse into the tissue, researchers can measure how effectively each one kills the patient’s cancer cells.
Such a device could eliminate much of the guesswork now involved in choosing cancer treatments, says Oliver Jonas, a postdoc at MIT’s Koch Institute for Integrative Cancer Research and lead author of a paper describing the device in the April 22 online edition of Science Translational Medicine.
“You can use it to test a patient for a range of available drugs, and pick the one that works best,” Jonas says.
The paper’s senior authors are Robert Langer, the David H. Koch Professor at MIT and a member of the Koch Institute, the Institute for Medical Engineering and Science, and the Department of Chemical Engineering; and Michael Cima, the David H. Koch Professor of Engineering at MIT and a member of the Koch Institute and the Department of Materials Science and Engineering.
Putting the lab in the patient
Most of the commonly used cancer drugs work by damaging DNA or otherwise interfering with cell function. Recently, scientists have also developed more targeted drugs designed to kill tumor cells that carry a specific genetic mutation. However, it is usually difficult to predict whether a particular drug will be effective in an individual patient.
In some cases, doctors extract tumor cells, grow them in a lab dish, and treat them with different drugs to see which ones are most effective. However, this process removes the cells from their natural environment, which can play an important role in how a tumor responds to drug treatment, Jonas says.
“The approach that we thought would be good to try is to essentially put the lab into the patient,” he says. “It’s safe and you can do all of your sensitivity testing in the native microenvironment.”
The device, made from a stiff, crystalline polymer, can be implanted in a patient’s tumor using a biopsy needle. After implantation, drugs seep 200 to 300 microns into the tumor, but do not overlap with each other. Any type of drug can go into the reservoir, and the researchers can formulate the drugs so that the doses that reach the cancer cells are similar to what they would receive if the drug were given by typical delivery methods such as intravenous injection.
After one day of drug exposure, the implant is removed, along with a small sample of the tumor tissue surrounding it, and the researchers analyze the drug effects by slicing up the tissue sample and staining it with antibodies that can detect markers of cell death or proliferation.
Ranking cancer drugs
To test the device, the researchers implanted it in mice that had been grafted with human prostate, breast, and melanoma tumors. These tumors are known to have varying sensitivity to different cancer drugs, and the MIT team’s results corresponded to those previously seen differences.
The researchers then tested the device with a type of breast cancer known as triple negative, which lacks the three most common breast cancer markers: estrogen receptor, progesterone receptor, and Her2. This form of cancer is particularly aggressive, and none of the drugs used against it are targeted to a specific genetic marker.
Using the device, the researchers found that triple negative tumors responded differently to five of the drugs commonly used to treat them. The most effective was paclitaxel, followed by doxorubicin, cisplatin, gemcitabine, and lapatinib. They found the same results when delivering these drugs by intravenous injection, suggesting that the device is an accurate predictor of drug sensitivity.
Read more: How to identify drugs that work best for each patient
The Latest on: Personalized medicine
[google_news title=”” keyword=”Personalized medicine” num_posts=”10″ blurb_length=”0″ show_thumb=”left”]
via Google News
The Latest on: Personalized medicine
- Researchers unveil digital 'alcohol twin' to predict drinking risks and guide personalized interventionson May 9, 2024 at 6:36 pm
By varying parameters such as body mass index (BMI), the model offers tailored insights into how specific drinking habits impact individuals differently, thereby enhancing its application in ...
- The Role of Data Science in Revolutionizing Personalized Medicine and Drug Discoveryon May 9, 2024 at 1:49 am
Genomic data holds immense promise in personalized medicine. Advances in DNA sequencing technologies have made it possible to decode an individual's entire genome, uncovering genetic variations that ...
- Global Companion Diagnostics Research Report 2024-2029: Innovations in Companion Diagnostics Boost Drug Development and Personalized Medicineon May 9, 2024 at 12:43 am
Factors such as the increasing importance of companion diagnostics in drug development, rising cancer incidence, and the growing adoption of targeted therapies are driving market growth.
- Biocartis and Merck to Collaborate on Improving Patient Access to Personalized Medicine in Middle East and North Africa (MEA) Regionon May 7, 2024 at 8:56 am
Biocartis (Mechelen, Belgium) announced an expansion of its collaboration with Merck Serono Middle East and Merck Saudi Ltd., both affiliates of Merck KGaA (“Merck”). The collaboration aims to improve ...
- OM1 Launches Three New Products Powered by Patented AI Platform to Expedite Delivery of Personalized Medicineon May 6, 2024 at 6:00 am
OM1 Orion, OM1 Lyra, and OM1 Polaris powered by PhenOMTM – an artificial intelligence-powered digital phenotyping platform for personalized medicine and clinical research. OM1 is the leader in ...
- Can a personalized antibiotics, prebiotics, and probiotics combo help treat IBS?on May 4, 2024 at 11:00 pm
A pilot study suggests that a personalized combination of antibiotics, prebiotics, and probiotics may help treat the symptoms of post-infectious irritable bowel syndrome (IBS).
- 'Despite promise, personalized medicine for head and neck cancers facing hurdles'on April 26, 2024 at 3:45 am
Improved efficacy: By identifying specific mutations driving tumour growth, personalized medicine allows for targeted therapies that have a higher success rate compared to ‘one-size-fits-all’ ...
- Translational Strategies to Implement Personalized Medicine: Rheumatoid Arthritis Exampleson April 18, 2024 at 5:00 pm
This gap between the rapidly increasing amount of disease-related genomic information and its clinical translation can be addressed through the creation and testing of personalized medicine ...
- Personalized Medicine in Oncologyon April 17, 2024 at 5:00 pm
Current advances in the biology of cancer and emergence of new tools for genome analysis have opened clinical perspectives in oncology, generally termed as 'personalized medicine'. This broad term ...
- Readers respond to OTC antidepressants, personalized medicine, restoring trust in public health, and moreon April 12, 2024 at 5:00 pm
This essay supports my assertion that the fiscal issues that might hinder the usefulness of personalized medicine need to be dealt with at the same time as we continue our progress towards large ...
via Bing News